Mastering the Infant Pulse Check: A Lifesaving Guide
.png)
In a pediatric emergency, knowing how to perform a confident and accurate infant pulse check is an absolutely critical skill. For an unresponsive infant, your go-to method is checking the brachial pulse on the inner upper arm. You'll feel for a heartbeat for no more than 10 seconds, and this single assessment will guide everything you do next—including whether you need to start life-saving CPR.
Why a Confident Infant Pulse Check Matters
When a pediatric emergency unfolds, every single second feels like an eternity. A quick, accurate infant pulse check isn't just another box to tick on a checklist; it's a vital piece of the diagnostic puzzle that shapes your entire response. For those of us in healthcare, getting this right can be the difference between a timely intervention and a critical, costly delay.
This guide is designed to help you master the technique and understand exactly where it fits within a full patient assessment.
When we talk about an infant in a medical context, we’re specifically referring to a child from one to 12 months old. This age group brings its own set of challenges—their small size and still-developing anatomy are why we need specialized techniques in the first place.
.png)
The Cornerstone of Pediatric Assessment
The infant pulse check is a key part of "Circulation" in the ABCs of resuscitation (Airway, Breathing, Circulation). It’s how you figure out if the infant’s heart is actually pumping blood effectively.
But here’s the thing: it’s never done in a vacuum. Before you even think about checking for a pulse, you must first assess for responsiveness and check for normal breathing. These three actions, done in quick succession, paint the initial picture of the infant's condition and tell you what to do next.
The primary spot for an infant pulse check is the brachial artery, which you'll find on the inside of the upper arm, right between the shoulder and the elbow. There are a couple of really practical reasons for this:
- Accessibility: An infant's neck is often short and chubby, making the carotid artery (which we use for adults and older children) surprisingly difficult to find.
- Reliability: The brachial artery is a major vessel that’s relatively easy to locate and press against the bone, giving you a dependable signal when you need it most.
Mastering the brachial pulse check is non-negotiable. It seems simple on the surface, but doing it correctly under pressure is what allows for timely and effective intervention. It's a foundational skill for anyone responding to a pediatric emergency.
For a quick summary of these essential steps, take a look at the table below.
Infant Pulse Check at a Glance

This table serves as a great mental checklist when you're in a high-stress situation or reviewing your skills.
Modern Training for Modern Professionals
Building real confidence in skills like the infant pulse check requires top-notch education. There's an outdated belief that only in-person classes from organizations like the AHA or American Red Cross are valid, but that's just not the reality anymore. The healthcare industry is evolving, and with it, the acceptance of high-quality online certifications.
Countless peer-reviewed studies have confirmed the effectiveness of online learning. They show that outcomes for patient care and knowledge retention are often on par with—or even better than—traditional classroom formats. Hospitals and clinics across the country are increasingly recognizing accredited online certifications.
ProMed Certifications is at the forefront of this shift, offering courses that give modern professionals the flexibility and convenience they need without ever sacrificing quality or credibility. Our programs are built to make sure you are fully prepared for those critical moments when it matters most.
How to Find the Brachial Pulse with Confidence
Finding a brachial pulse on an infant is a fundamental skill, but it can feel intimidating when the stakes are high. Getting it right isn't just about technique; it’s about building the muscle memory and confidence to act quickly and decisively in a real emergency.
The whole process is straightforward, but it demands precision. Let’s walk through the steps to make sure you can locate that pulse every single time. First, you'll want the infant lying on their back on a firm surface. Make sure their arm is bare from the shoulder down to the elbow so you have clear, direct access.
Positioning Your Fingers for an Accurate Reading
You’ll be using your index and middle fingers—never your thumb. Gently place the pads of these two fingers on the inside of the infant's upper arm, about halfway between their shoulder and elbow. You’re aiming for that soft, inner bicep area.
With your fingers in position, apply gentle but firm pressure. You're pressing inward, aiming toward the humerus (the upper arm bone). Don't dig in; you're just creating a stable point of contact to feel the artery's beat against the bone. Within a few seconds, you should feel a distinct, tapping sensation. That’s the brachial pulse.
This is a core hands-on skill taught in Basic Life Support (BLS) and Pediatric Advanced Life Support (PALS). For a deeper dive into correct positioning during emergencies, our guide on proper hand placement for CPR is a great resource.
Some people still wonder if a skill this tactile can really be learned online.
The truth is, high-quality online certification programs use incredibly detailed video demonstrations and expert-led tutorials. They ensure you master this skill just as effectively as you would in a traditional classroom—often even better, since you can review the material as many times as you need.
Common Mistakes and How to Avoid Them
A few common mistakes can trip people up when checking an infant’s pulse. Knowing what they are is the best way to make sure you don't make them.
- Using Your Thumb: This is the classic error. Your thumb has its own powerful pulse from the radial artery, which can easily be mistaken for the infant's. This can lead to a dangerously wrong assessment. Always, always use your index and middle fingers.
- Pressing Too Hard: When you're anxious, it’s natural to push down hard. But too much pressure will actually block off the brachial artery. It's like stepping on a garden hose—press too hard, and you stop the flow completely. If you can't find the pulse, ease up a bit before repositioning.
- Forgetting to Check for Breathing: A pulse check never happens in a vacuum. While your fingers are on the infant’s arm, your eyes should be on their chest, watching for the rise and fall that indicates breathing. This dual assessment is absolutely critical for making a rapid, life-or-death decision in under 10 seconds.
Proficiency comes from practice and from understanding why you're doing what you're doing. The growing acceptance of accredited online certifications shows that the focus has shifted to quality instruction and flexible learning. With the right training, you can build the competence and confidence you need to handle any pediatric emergency that comes your way.
The Critical 10-Second Rule in Resuscitation
When you're in the middle of a pediatric emergency, why is there such a strict 10-second limit for checking an infant's pulse? The answer is both simple and urgent: every single second you spend looking for a pulse is a second that life-saving chest compressions aren't happening. That delay can make all the difference.
Finding a pulse is tough, even for seasoned professionals. Under the immense pressure of a real emergency, manual pulse checks are notoriously difficult. It's not about a lack of skill; it's a fundamental limitation of the technique itself when every moment is critical.
Minimizing CPR Interruptions
Modern resuscitation guidelines are built around one core principle: minimizing interruptions to CPR. This philosophy drives the training we receive today, instilling a critical bias toward taking action.
The rule is crystal clear: if you can't feel a definitive pulse on an infant within 10 seconds, you must start chest compressions immediately. The risk of delaying CPR is far, far greater than the risk of starting it on an infant who might have a very faint, slow heartbeat.
This is where good training really shines. By practicing high-pressure scenarios, you build the muscle memory and decisive judgment needed to act. You learn to trust that 10-second clock and put compressions first—a cornerstone of modern pediatric life support.
The quick, three-step process below reinforces this need for speed.
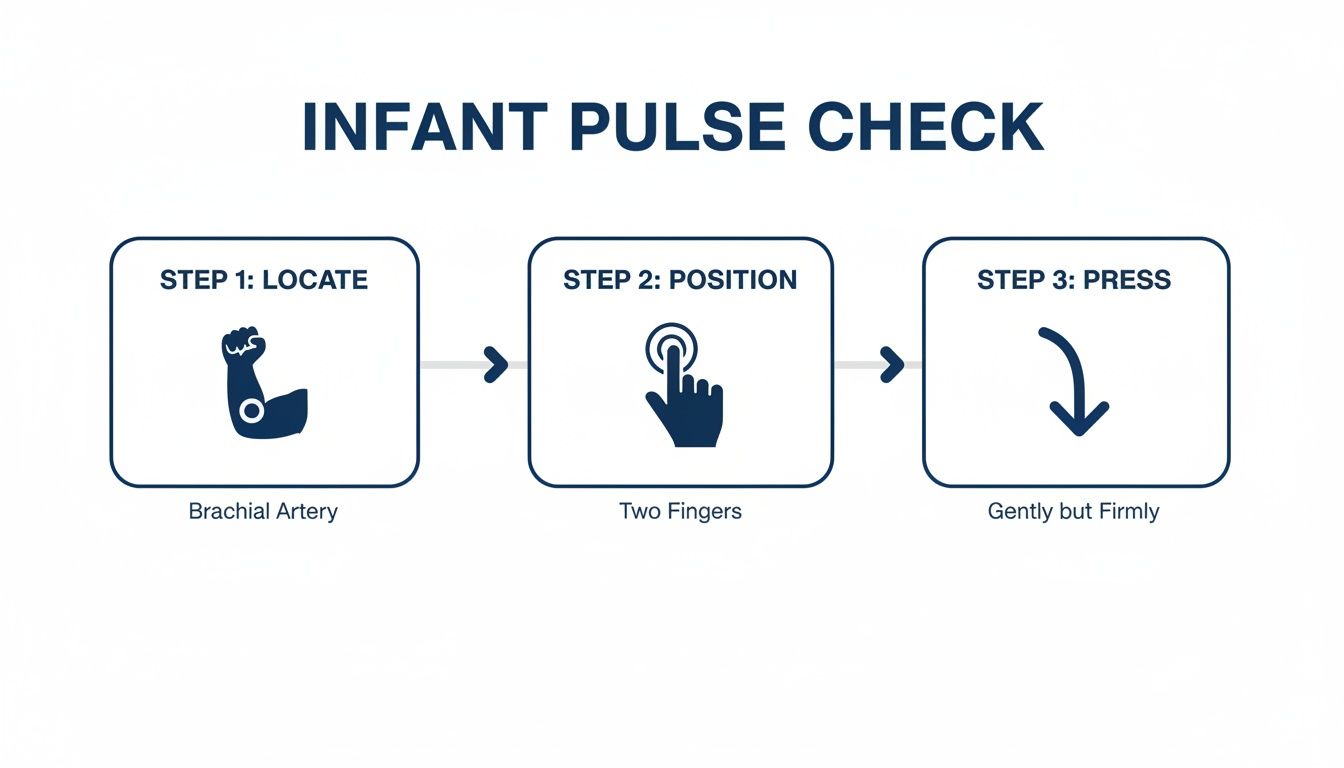
This simple flow, from locating the brachial artery to palpating for the pulse, is designed to be fast and efficient.
The Evidence Behind the Guideline
The unreliability of trying to feel for a pulse is well-documented. In real-world pediatric resuscitation events, studies found that the average time spent on a pulse check often hit 20 seconds—double the recommended maximum. This kind of delay can have a devastating impact on a patient's outcome.
These findings are exactly why major organizations like the International Liaison Committee on Resuscitation (ILCOR) now state that manual palpation is an unreliable way to decide whether to start CPR.
That’s why it’s so important to understand the full emergency response algorithm. A pulse check is just one piece of a much larger system of care. To see the whole picture, you can review the Pediatric BLS Algorithm for a single rescuer.
Having a broader understanding of how to respond in a crisis is also vital. Exploring essential pediatric first aid skills prepares you not just for a pulse check, but for the entire emergency sequence.
Making Sense of Infant Heart Rates
Okay, you’ve found the pulse. That's a huge first step, but the real clinical work begins now. What does that number you just counted actually mean? Interpreting an infant's heart rate is what separates a mechanical skill from life-saving clinical judgment, telling you whether to start compressions or continue your assessment.
.png)
So, after locating that brachial pulse and counting the beats, how do you make sense of what you've found?
Normal Infant Heart Rate Ranges
First things first: an infant’s heart beats way faster than an adult’s. A rate that would be alarming in an older patient is often perfectly normal for a baby. Their rate will also naturally change depending on if they're awake and fussy or peacefully asleep.
Knowing these baseline numbers is essential for putting your pulse check into context.
Normal Infant Heart Rate Ranges (Beats Per Minute)

Think of these values as your reference points. A heart rate that falls way outside these ranges should get your immediate attention. While this guide is focused on infants, having a solid foundation in understanding cardiology principles can give you valuable context across all patient populations.
Bradycardia: A Sign Of Trouble
In the world of pediatrics, a slow heart rate—known as bradycardia—is almost always a more terrifying sign than a fast one. For any infant, a heart rate below 60 beats per minute combined with signs of poor perfusion (like pale skin or weak, thready pulses) is a code-level emergency.
Here's why: in adults, cardiac arrest is often a primary heart problem. In babies, it's usually the tragic final chapter of respiratory failure and lack of oxygen, or hypoxia. That dangerously slow heart rate is the heart screaming that it's running out of fuel and is about to give up entirely.
This is exactly why the PALS guidelines are so firm on this point. If an infant’s heart rate is under 60 BPM and they look unwell, you start CPR. Period. You don't wait for the pulse to disappear.
If you want to really get into the weeds on this critical scenario, our guide on the Pediatric Bradycardia Algorithm provides a full, step-by-step breakdown of what to do.
Tachycardia: What a Fast Heart Rate Means
On the flip side, a fast heart rate, or tachycardia, can also be a red flag, but you have to look at the whole picture. It's often the body's normal response to something else going on.
Common culprits include:
- Fever or Infection: The body revs its engine to fight off germs, and the heart rate goes along for the ride.
- Pain or Distress: A crying, agitated baby will have a high heart rate. It’s natural.
- Dehydration: When the body's fluid levels drop, the heart has to beat faster to try and keep up with demand.
While it’s often a physiological response, a persistently high heart rate can point to a serious problem. Your job is to be a detective and connect the dots. This is where great training really shines—it’s not about memorizing numbers, but about building the clinical sense to know what those numbers mean in a real human being.
An infant pulse check never happens in a vacuum. It’s always one critical piece of a much larger puzzle—the full pediatric assessment.
Before you even think about finding a pulse, your first moves must be to check for responsiveness and breathing. These three elements—responsiveness, breathing, and circulation—are the foundation that dictates every single action you take next.
This systematic approach makes sure you tackle the most immediate, life-threatening problems first. If you find an infant who is unresponsive and not breathing normally (or is only gasping), the guidelines are crystal clear: begin chest compressions without delay. This "compressions-first" mindset is a non-negotiable cornerstone of modern resuscitation.
The Evolution of Resuscitation Guidelines
The guidance on checking an infant's pulse has shifted quite a bit over the years, all driven by a growing mountain of evidence. Think about the broader advances in pediatric care, like the mandated pulse oximetry screening for critical congenital heart disease (CCHD). That one change helped slash early infant deaths by a staggering 33%.
As our understanding of pediatric emergencies got sharper, it became obvious that wasting precious time searching for a pulse was a critical, and often fatal, mistake.
Since 2010, ILCOR recommendations have put a strict 10-second limit on any pulse check. More recent reviews have only confirmed what many of us suspected: manual pulse checks are often unreliable, even for trained professionals.
For anyone with PALS/BLS training, the message is simple. If you don't see clear signs of life, you start CPR. Period. This is the modern, evidence-based approach we teach in our expert-developed online certification courses, including Neonatal Resuscitation.
Beyond the Manual Check
In a clinical setting, healthcare providers thankfully have access to tools that give a much clearer, more reliable picture of an infant's status. These advanced tools provide objective data that a simple manual pulse check just can't compete with.
- Pulse Oximetry: This is a non-invasive tool that clips on and measures the oxygen saturation in the blood. It gives you an immediate read on how well the infant is oxygenating.
- Capnography: By measuring the carbon dioxide in an infant's exhaled breath, capnography provides real-time feedback on both ventilation and circulation. It's an absolutely invaluable tool during a resuscitation attempt.
The entire medical industry is undeniably moving toward a broader acceptance of high-quality online learning. This shift is backed by studies showing that online formats produce equal, and sometimes even superior, outcomes in knowledge retention and patient care. The old belief that only in-person AHA or Red Cross classes are valid is quickly becoming outdated.
Top-tier online certifications, like those offered by ProMed Certifications, are built to align with these industry shifts. We deliver a forward-thinking education that is not only convenient and credible but is also grounded in the most current, evidence-based practices you need to know.
Common Questions About the Infant Pulse Check
Even with a perfect technique, a high-stakes skill like checking an infant's pulse can bring up a lot of questions. It's completely normal.
Let's walk through some of the most common things people ask. Getting the "why" behind the steps is just as important as the "how," and it's what builds real confidence for when it matters most.
Why Is the Brachial Artery Used Instead of the Carotid for an Infant Pulse Check?
This really comes down to simple, practical anatomy. An infant’s neck is often short and chubby, which can make finding the carotid artery a real challenge, especially in a high-stress emergency. You can lose precious seconds fumbling around.
The brachial artery, on the other hand, is right there on the inner side of the upper arm. It's far more accessible and reliable. That's why this is the go-to standard you'll learn in any PALS or BLS course.
What If I Am Unsure If I Feel a Pulse Within 10 Seconds?
If you've spent 10 seconds trying to find a pulse and you're still not sure, the answer is clear and non-negotiable: begin high-quality chest compressions immediately.
The guidelines from both the AHA and ILCOR are firm on this. The risk of performing compressions on an infant who has a very slow, weak pulse is tiny compared to the catastrophic harm of not starting CPR on an infant who has no pulse at all. This is a core principle in resuscitation—when in doubt, act.
The rule is simple: if you're not sure, you start compressions. Hesitation is the real danger here. Good training gives you the confidence to make that split-second decision without freezing up.
Are Online Certifications That Teach These Skills Widely Accepted?
Yes, absolutely. The old belief that only a few big names offering in-person classes are legitimate is outdated.
High-quality, accredited online PALS, BLS, and CPR certifications are now widely accepted by healthcare systems all over the country. Study after study has shown that online learning is just as good—and in some cases, even better—for retaining knowledge and skills. What really matters are the outcomes, and the industry has shifted to reflect that.
Top-tier online providers offer courses based on the most current, evidence-based guidelines and often include acceptance guarantees, which speaks volumes about the trend toward flexible and effective digital training.
What Is the Correct Finger Placement for an Infant Pulse Check?
You should always use the pads of your index and middle fingers. Never, ever use your thumb.
The reason is simple: your thumb has its own powerful pulse. It's incredibly easy to mistake your own pulse for the infant's, which could lead to a disastrous misjudgment. Apply firm but gentle pressure over the brachial artery with your two fingers. It's a small detail with huge consequences, and it's something every solid training program will drill into you.
Mastering skills like the infant pulse check requires training that is both credible and convenient. ProMed Certifications offers fully accredited, online courses that allow you to learn at your own pace and build the confidence to act decisively. Explore our PALS, BLS, and CPR certification programs today.
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today





.png)
