What Is Neonatal Resuscitation A Guide to Life-Saving Newborn Care

At its core, neonatal resuscitation is a series of immediate, life-saving actions taken when a newborn struggles to breathe on their own right after birth. Think of it as providing a gentle but absolutely critical "jump-start" to a baby's breathing and circulatory systems. This isn't some rare, dramatic event; it's one of the most vital procedures performed in delivery rooms worldwide, with a direct line to newborn survival. This guide will help you understand the core principles, the step-by-step process, and how you can get certified with modern, effective training.
Understanding Neonatal Resuscitation and Its Critical Importance
When a baby takes its first breath, it’s making a monumental transition from the quiet, fluid-filled world of the womb to breathing air. For most newborns, this switch happens instinctively. But for some, that first breath doesn't come easily, and that's precisely where neonatal resuscitation steps in. The entire process follows a carefully structured algorithm designed to stabilize the baby quickly and effectively.
To ensure every action is rooted in the most current medical science, the fundamental principles of neonatal resuscitation are constantly being refined based on comprehensive Evidence Based Practice Guidelines.
The Goals of Resuscitation
The primary mission is to prevent birth asphyxia—a dangerous lack of oxygen to the brain and other organs—which can lead to devastating, long-term complications. The immediate goals are straightforward but incredibly urgent.
To help break this down, here’s a quick overview of the main objectives:
Key Goals of Neonatal Resuscitation

Achieving these goals is the foundation of giving a struggling newborn the best possible start.
The global impact of effective resuscitation is massive. Tragically, in 2020, 2.4 million newborns died within their first 28 days, with birth asphyxia being a major contributor. The good news? High-quality training in neonatal resuscitation can slash these asphyxia-related deaths by up to 30%. If these skills were universally available, it could potentially save nearly two million lives every single year.
Of course, the first step in any resuscitation is a rapid assessment of the newborn's condition. A key tool for this is the APGAR score. You can check out our guide on how to use the APGAR score to understand how this quick evaluation works.
Navigating the Neonatal Resuscitation Algorithm
Think of the Neonatal Resuscitation Program (NRP) algorithm less like a rigid checklist and more like a dynamic roadmap. It's designed to keep you clear-headed and decisive during the critical first moments of a newborn's life, guiding you from assessment to action with precision.
It all boils down to three simple, yet incredibly powerful, questions you must ask the second the baby is born:
- Is the baby term?
- Does the baby have good muscle tone?
- Is the baby breathing or crying?
The answers to these questions are your immediate fork in the road. If you can answer "yes" to all three, the baby is generally fine and can stay with the mother for routine care—drying, skin-to-skin contact, and just keeping a close eye on them.
But if the answer to any of those is "no," the algorithm kicks in, pointing you toward the initial steps of resuscitation.
The Initial Steps of Stabilization
When a newborn needs a helping hand, the first moves are all about the basics: providing warmth, making sure the airway is clear, and stimulating the baby to breathe.
This usually just means drying the infant off vigorously and repositioning their head to open up the airway. More often than not, these simple actions are all it takes to get a baby to take their first effective breaths.
If these initial steps don't lead to good breathing and a heart rate above 100 beats per minute, the algorithm guides you to the next level: positive-pressure ventilation (PPV). This is a crucial pivot point where breathing for the baby becomes the number one job.
Advancing Through the Algorithm
Neonatal resuscitation happens on a massive scale. Up to 16% of the world's 140 million annual newborns need some kind of help to get started.
That’s why the guidelines from the American Heart Association (AHA) and American Academy of Pediatrics (AAP) are always being refined. Recent updates, for instance, have put a bigger spotlight on delayed cord clamping and the power of non-invasive PPV, which is needed in up to 12% of all births. This really drives home how vital it is to have a clear, step-by-step path to follow.
The decision tree below shows exactly how a provider moves from that first quick look to deciding if a newborn is doing fine or needs help.
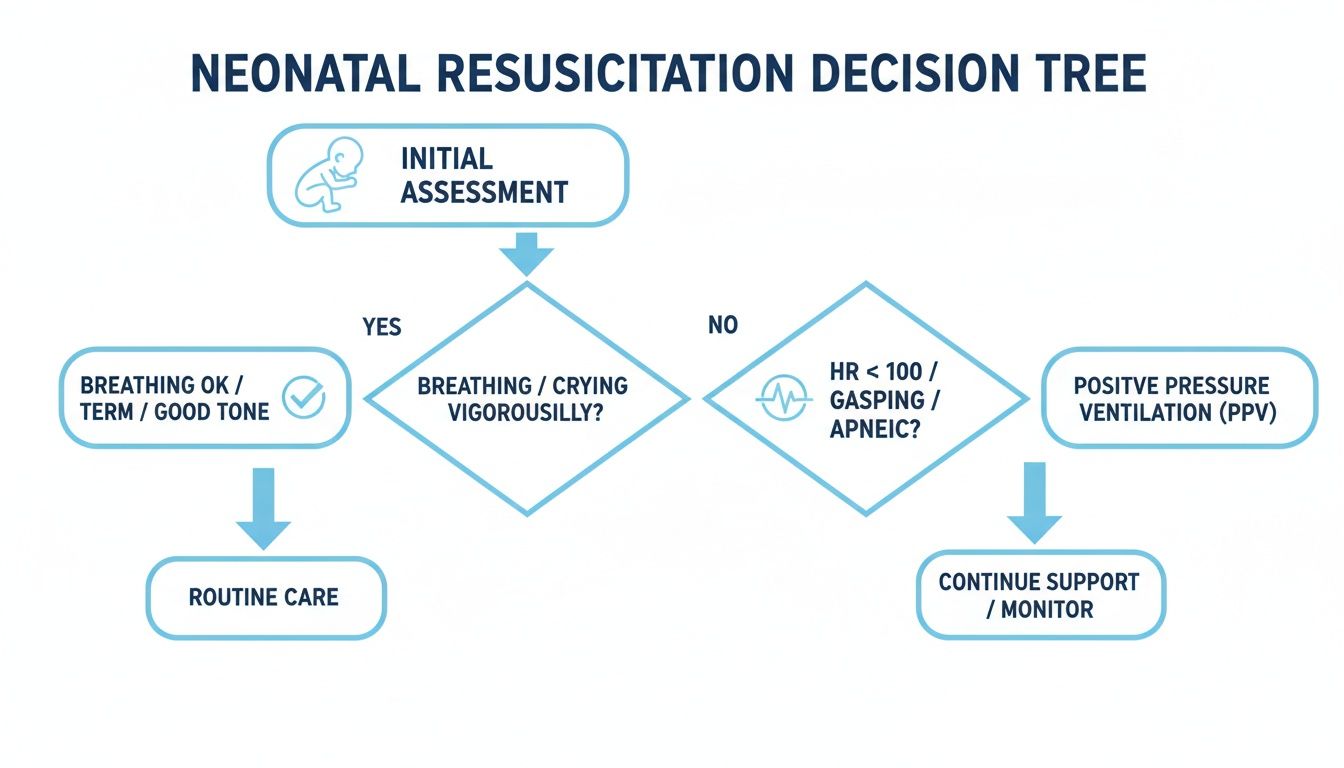
This visual really clarifies how the answers to those first three questions send you down one of two paths: routine care or the resuscitation sequence.
If PPV doesn't get the heart rate up, the algorithm has your next move ready. You'll be prompted to double-check your ventilation technique, think about placing an advanced airway, and eventually, start chest compressions coordinated with breaths.
Medications like epinephrine are saved for last, used only when the heart rate stays critically low despite solid ventilation and compressions. Each step flows logically from the last, ensuring you do the right things in the right order. Getting this flow down is what high-quality training is all about. You might be interested in a more detailed look at the specifics of neonatal algorithms and how they guide care.
Mastering Core Resuscitation Interventions
The neonatal resuscitation algorithm gives you the "when," but the hands-on interventions are the "how." These are the core techniques that form the heart of the life-saving process, turning knowledge into direct, effective action. Each step is a practical skill designed to address a specific physiological need, from maintaining body temperature to ensuring the baby is breathing and their heart is pumping.
Let’s break down the essential actions you'll learn and practice to prepare for these critical moments. The goal here is to make these procedures feel less intimidating and more like a set of clear, manageable steps—reinforcing why regular, high-quality training is so vital.

Warming and Initial Stimulation
A newborn, especially one in distress, can lose body heat with alarming speed. That's why the very first actions are always about getting the baby warm and dry.
- Drying and Warming: The baby is immediately placed under a radiant warmer and dried thoroughly with warm blankets. This simple act of removing wet amniotic fluid prevents rapid heat loss and provides gentle stimulation.
- Stimulation: Sometimes, all it takes is rubbing the baby’s back and flicking the soles of their feet to encourage that first crucial cry and establish regular breathing.
Often, these initial steps are all that’s needed to help a newborn make a successful transition. If not, the team moves swiftly to support the airway.
Airway Positioning and Suctioning
An open airway is non-negotiable for effective breathing. Think of it like making sure a garden hose is straight and unblocked before you turn on the water.
The baby is placed on their back with their head in a "sniffing position"—neck slightly extended—which aligns the airway perfectly. If there are obvious secretions blocking the mouth or nose, gentle suctioning with a bulb syringe or suction catheter clears the path for air to get to the lungs.
Key Insight: Overly aggressive suctioning can cause a reflex slowing of the heart rate (bradycardia), so the technique has to be gentle and quick. Always clear the mouth before the nose.
Positive-Pressure Ventilation
When a newborn's breathing is ineffective or absent despite initial stimulation, positive-pressure ventilation (PPV) is the next critical step. This is where you deliver breaths to the baby using a bag-mask device.
Effective PPV is a skill. It requires a precise technique to create a good seal around the baby’s nose and mouth and deliver breaths at the correct rate—about 40 to 60 breaths per minute. The goal is to see a visible rise in the baby’s chest with each breath, which confirms that air is actually entering the lungs.
Chest Compressions and Medications
If the baby's heart rate drops below 60 beats per minute despite 30 seconds of effective PPV, it's time to start chest compressions. The technique involves using two thumbs to depress the sternum, coordinated with ventilations in a 3:1 ratio—that’s three compressions for every one breath.
Medications, primarily epinephrine, are reserved for those rare situations where the heart rate just won't respond to effective ventilation and coordinated compressions. It's administered to help stimulate the heart and improve blood flow.
Mastering these interventions is what neonatal resuscitation certification is all about. Building this hands-on confidence is achievable through dedicated practice, which is why flexible and accessible training like the Neonatal Resuscitation course offered by ProMed Certifications is so important for today’s busy healthcare professionals.
Choosing Your Neonatal Resuscitation Certification
When it comes to a skill as critical as neonatal resuscitation, picking the right certification path is a big deal. For a long time, there was an outdated belief that only in-person courses from specific organizations like the AHA or American Red Cross were valid. This is simply not true anymore, and the healthcare world is embracing smarter, more efficient training methods.
Today, accredited online certifications aren't just an alternative; they are a widely respected and effective option. Hospitals, clinics, and healthcare systems across the country are increasingly recognizing their validity. The industry is evolving, understanding that quality education is about the curriculum and outcomes, not the delivery format.
The Shift Toward Online Learning
The move to online education is about more than just convenience; it’s backed by solid evidence. Many peer-reviewed studies and industry articles have shown that online learning can lead to equal or even superior knowledge retention and patient care outcomes compared to traditional classrooms. You can absorb complex information at your own pace, rewind a tricky module, and review materials until you genuinely feel you've mastered them.
This flexibility is a game-changer. Instead of rearranging your work schedule and personal life to sit in a rigid, day-long class, you can weave your certification training into your existing routine. It's a modern, future-focused approach that respects your time while delivering the high-caliber education you need to save lives.
The general consensus in the industry is shifting. Healthcare organizations are realizing that what truly matters is the quality of the education and its alignment with the latest guidelines—not the format it's delivered in.
Comparing Training Formats
When you put the two options side-by-side, the advantages of a modern online program really stand out. While in-person classes can offer hands-on practice, they often come with logistical challenges and costs that are tough for a working professional to navigate.
To give you a clearer picture, we've put together a quick comparison. This table breaks down the key differences between earning your certification online with a provider like ProMed versus attending a traditional, scheduled class.
Comparing Online vs In-Person Neonatal Resuscitation Training

As you can see, the flexibility, efficiency, and equal quality of online learning make it a powerful choice for today's healthcare providers.
Ultimately, the goal is to build your competence and confidence in handling one of the most stressful situations in medicine. At ProMed Certifications, we're proud to be at the forefront of this educational shift, offering a credible, convenient, and forward-thinking path to certification. Our courses are built to empower you with essential skills, on your own terms.
Learn more about how you can get your accredited Neonatal Resuscitation certification online and join the thousands of professionals who trust our modern approach to medical education.
Practical Strategies for Resuscitation Success
Knowing the neonatal resuscitation algorithm is one thing. Executing it flawlessly under pressure is a completely different ballgame. Real success comes down to preparation, teamwork, and crystal-clear communication. Let’s go beyond the textbook steps and talk about the practical strategies that make a good team great in those critical moments.

These are the habits that sharpen a team’s performance, slash the risk of errors, and ultimately give every newborn the best possible start.
Before the Event: Pre-Delivery Briefings
The best resuscitations start before the baby is even born. A quick, focused pre-delivery briefing is your team's most powerful tool for getting ready. This is where you anticipate potential problems, double-check your equipment, and assign clear roles to every single person on the team.
Think of it like a huddle before a big play in sports. Everyone needs to know their exact job—who’s on the airway, who starts chest compressions if needed, and who’s documenting everything? Nailing this down beforehand eliminates deadly hesitation when the clock is ticking.
During the Event: Closed-Loop Communication
In the chaos of a delivery room, communication can break down fast. This is why top-performing teams rely on closed-loop communication. It's a simple technique, but it’s incredibly powerful for preventing mistakes.
Here’s the breakdown:
- Give a Clear Order: The team leader says something specific, like, "Sarah, please prepare a 0.1 mg/kg dose of epinephrine."
- Confirm the Order: The team member repeats it back to show they understood. "Got it. Preparing 0.1 mg/kg of epinephrine."
- Announce Completion: Once the task is finished, they close the loop. "The epinephrine is drawn up and ready."
This simple back-and-forth ensures every instruction is heard, understood, and acted on, which drastically cuts down on errors.
Key Takeaway: Neonatal resuscitation is a team sport. Individual skill is vital, but synchronized, collaborative effort is what truly drives successful outcomes.
Given that neonatal resuscitation is such a team-based effort, understanding the principles of collaborative learning can seriously boost training effectiveness and how well the team functions during an actual emergency.
After the Event: Post-Event Debriefings
The learning isn't over just because the resuscitation is. A quick, blame-free debriefing afterward is essential for getting better. This gives the team a chance to talk about what went right, what was challenging, and what could be done differently next time.
This habit builds a stronger, more cohesive team and turns every experience, good or bad, into a valuable lesson. It reinforces that competence isn't a finish line; it's a constant journey of learning and sharpening your skills. This commitment to staying ready is exactly why accessible online recertification, like the programs offered by ProMed, is so important. It gives you a straightforward way to keep your knowledge fresh, ensuring you’re always prepared to perform at your best.
Your Top Neonatal Resuscitation Questions Answered
When you're dealing with a skill as critical as neonatal resuscitation, it's only natural to have a few questions. Let's walk through some of the most common ones we hear from healthcare professionals to clear up any confusion and bust a few myths about certification.
Who Really Needs This Certification?
Simply put, if your job could put you in the room during labor, delivery, or the moments just after a baby is born, this certification is for you. It's for any healthcare provider who might be called on to help a newborn breathe.
This isn't just for specialists. The list is long and includes:
- Obstetricians, pediatricians, and neonatologists
- Family physicians and nurse midwives
- Labor and delivery nurses and NICU staff
- Respiratory therapists
- Emergency medical personnel
If you're on the front lines of welcoming new life into the world, you need to be prepared. This training ensures you can act with confidence when it matters most.
How Often Do I Need to Renew My Certification?
The standard across the healthcare industry is to renew your neonatal resuscitation certification every two years. This isn't just an arbitrary timeline; it's designed to keep your skills sharp and your knowledge current with the latest guidelines from key organizations like the American Academy of Pediatrics (AAP).
Think of it as a professional responsibility. These are high-stakes, low-frequency skills for many providers. Regular recertification keeps them fresh in your mind. Thankfully, modern online platforms make it easy to fit this renewal into a packed schedule, saving you the headache of coordinating in-person classes.
Are Online Neonatal Certifications Actually Accepted by Employers?
Yes, absolutely. The outdated belief that only legacy providers like the AHA or American Red Cross offer valid certifications is no longer accurate. High-quality, accredited online certifications are now widely accepted by hospitals, clinics, and healthcare systems everywhere as the industry evolves.
The reality is that the healthcare industry has embraced online learning as a highly effective and practical way to maintain essential skills.
The consensus is clear and continues to grow: many peer-reviewed studies show that for knowledge retention and patient care outcomes, online learning formats are just as good, if not better, than their in-person counterparts.
Providers like ProMed Certifications build their courses on the most current ILCOR and AAP guidelines and even back them with a 100% acceptance guarantee. This gives you peace of mind, knowing your training is credible, respected, and will be recognized by your employer.
How Is This Course Different from the NRP?
This is an excellent and very important question. The Neonatal Resuscitation Program, or NRP, is a specific, branded program from the AAP and AHA. A key part of their process is often a mandatory in-person skills session.
A general neonatal resuscitation course, like the one we offer at ProMed Certifications, covers the exact same cognitive knowledge and algorithmic decision-making. Our curriculum is built on the very same evidence-based guidelines, giving you the critical theoretical foundation you need. Our course is a valid and accepted certification option for many employers, providing a more flexible and accessible way to keep your life-saving skills up to date.
At ProMed Certifications, our goal is to provide credible, convenient, and forward-thinking education that fits the lives of modern healthcare professionals. Ready to get certified or renew your credentials without the hassle? Take a look at our fully accredited Neonatal Resuscitation course and take control of your professional development today.
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today