Bloodborne Pathogens Precautions: Your 2026 Safety Guide
.png)
In any clinical setting, some of the biggest risks are the ones you can't even see. That's why bloodborne pathogens precautions are more than just a chapter in a training manual—they are the bedrock of safety measures that every healthcare professional must master to prevent exposure to infectious microorganisms in human blood. Think of them as a non-negotiable part of your daily routine, protecting you from threats like HIV, Hepatitis B (HBV), and Hepatitis C (HCV). This guide will help you master the essential precautions to keep yourself, your colleagues, and your patients safe.
What Are Bloodborne Pathogens and Why They Matter

Think of bloodborne pathogens as microscopic stowaways—dangerous organisms that travel in blood and other body fluids. For the nearly 18 million healthcare workers in the United States, this isn't a distant threat; it’s a potential reality of the job. Getting a firm grip on what these pathogens are and the serious diseases they can cause is the absolute first step toward keeping yourself safe.
The most common culprits you'll hear about are:
- Hepatitis B Virus (HBV): A serious liver infection that, thankfully, can be prevented with a very effective vaccine.
- Hepatitis C Virus (HCV): Another virus that attacks the liver, which can lead to chronic disease and severe long-term damage.
- Human Immunodeficiency Virus (HIV): The virus responsible for Acquired Immunodeficiency Syndrome (AIDS), which cripples the body's immune system.
And these aren't the only ones. Less common but equally dangerous pathogens, like the Ebola virus, can also spread through blood. This is precisely why mastering bloodborne pathogens precautions is so critical.
Understanding Transmission Risks
Exposure happens when infected blood or other materials find a way into your body. This doesn't have to be a dramatic, movie-style splash. Most exposures are far more subtle and can happen through common pathways you encounter every day in a healthcare environment.
Think of it like this: a tiny, unseen break in your skin is like an open door for these pathogens. Even minor skin conditions like acne, chapped skin, or a papercut can create an entry point.
A needlestick is the classic example, but exposure isn't limited to sharps injuries. It can also happen when infectious materials come into contact with:
- Mucous membranes in your eyes, nose, or mouth.
- Non-intact skin, including any cuts, burns, or rashes.
- A puncture from any contaminated sharp, like a scalpel, broken glass, or needle.
You'll also need to know the term Other Potentially Infectious Materials (OPIM). It's a wide-ranging category that covers fluids like semen, vaginal secretions, and cerebrospinal fluid, as well as any body fluid that has visible blood in it.
Since it's often impossible to tell just by looking whether a patient is infectious, your best defense is to treat all human blood and OPIM as if they are. This fundamental rule is the heart of Standard Precautions. Internalizing this mindset doesn't just protect you—it protects your colleagues and the very patients you're dedicated to helping.
The OSHA Standard That Keeps You Safe
For anyone in healthcare, workplace safety isn't just a corporate buzzword—it's a real, tangible part of your day-to-day. The foundation of that safety is the Occupational Safety and Health Administration (OSHA) Bloodborne Pathogens Standard, officially known as 29 CFR 1910.1030.
This isn't just another dusty rulebook. Think of it as a powerful shield, a set of guarantees designed to protect you from exposure to infectious materials on the job.
It’s hard to imagine now, but before this standard was introduced in 1991, healthcare was a far riskier field. Nurses, doctors, and lab techs were constantly exposed to dangerous pathogens from needlesticks and splashes, often with little to no formal protection from their employers.
The OSHA standard changed everything, turning workplace safety into a legal requirement. The results were dramatic. Hepatitis B infections among healthcare workers, for example, plummeted after employers were required to provide free vaccinations.
But the fight isn't over. The CDC estimates that U.S. hospitals still see nearly 400,000 needlesticks every year. That number almost doubles when you factor in other healthcare settings. It’s a stark reminder that we can never let our guard down. For a deeper look at the history and risks, the NYSNA website offers some powerful context.
What Your Employer Is Required to Do
Understanding this standard is crucial because it spells out exactly what protections your employer legally owes you. It takes safety from a nice idea and makes it a non-negotiable part of your work environment.
Here are the core responsibilities your employer must fulfill:
- Create and Maintain an Exposure Control Plan (ECP): This is a living document, a written plan detailing how your specific workplace prevents exposures. It has to be updated every year and be available for you to review anytime.
- Provide Free Hepatitis B Vaccinations: If your job puts you at risk of exposure, your employer must offer you the complete Hepatitis B vaccine series, completely free of charge.
- Supply All Necessary Personal Protective Equipment (PPE): This isn't optional. Your employer must provide gloves, gowns, face shields, masks, and any other required PPE, and make sure you know how to use it properly.
- Use Engineering and Work Practice Controls: This means providing safer equipment, like sharps disposal containers and self-sheathing needles, and enforcing safe habits, like proper handwashing.
- Offer Post-Exposure Follow-Up: If you do have an exposure incident, your employer is required to provide a confidential medical evaluation and any necessary follow-up care at no cost to you.
How This Empowers You
At its heart, the OSHA standard gives you specific rights and a clear playbook for staying safe. You have the right to get annual training, the right to see your workplace's ECP, and the right to have all the safety gear you need to do your job.
Knowing these rules lets you take an active role in your own safety. It gives you the confidence to spot problems, ask for the right equipment, and stick to procedures that protect both you and your patients.
Ultimately, the standard creates a partnership. Your employer provides the safe environment, the tools, and the training. Your job is to use them consistently and correctly. This shared responsibility is what makes these precautions so effective at minimizing risk and building a true culture of safety.
How To Apply Universal And Standard Precautions
In healthcare, we operate on a simple but powerful rule: treat all human blood and certain body fluids as if they're infectious. This is the bedrock of Universal Precautions and the newer, more comprehensive Standard Precautions.
Think of it as the "defensive driving" of medicine. You don't wait to see if a patient has a known infection; you anticipate the risk in every interaction to keep yourself and others safe.
This mindset is absolutely critical. In the U.S. alone, an estimated 18 million healthcare workers are at risk of occupational exposure to pathogens like HIV, HBV, and HCV. Studies show nurses are hit hardest, accounting for 63% of all exposure incidents. With sharps injuries being a top mode of transmission, these precautions are a daily, non-negotiable part of the job. For a deeper look at these on-the-job hazards, the OSHA website provides extensive details.
The Shift From Universal To Standard Precautions
The concept of Universal Precautions (UP) emerged back in the 1980s, primarily to combat the spread of HIV. It was a huge step forward, establishing the baseline practice of using barriers like gloves when handling blood and specific body fluids.
But as our understanding of infection control evolved, we realized we needed a broader shield.
In 1996, the CDC introduced Standard Precautions (SP). This wasn't a replacement for Universal Precautions but an evolution that merged its principles with another concept called Body Substance Isolation (BSI).
The key difference is scope. UP was laser-focused on blood. Standard Precautions, on the other hand, apply to all patient care, assuming potential risk from:
- All blood and body fluids (except sweat), whether blood is visible or not
- Non-intact skin like cuts, rashes, or abrasions
- Mucous membranes (your eyes, nose, and mouth)
This wider net protects you from both known and hidden infection risks in every single patient encounter.
To make the distinction crystal clear, it helps to see how these two frameworks compare. Universal Precautions laid the groundwork, but Standard Precautions built a much more robust structure on top of it.
Universal Precautions vs. Standard Precautions

In short, Standard Precautions became the new "gold standard" by making safety measures a universal habit, not just a response to visible blood.
Core Practices Of Standard Precautions
Putting Standard Precautions into action isn't about memorizing a list; it's about building a routine of safety that becomes second nature. These habits are the building blocks of any effective infection control program.
- Meticulous Hand Hygiene: This is, without a doubt, the single most important practice. You must wash your hands with soap and water or use an alcohol-based hand sanitizer before and after every patient contact, after taking off gloves, and anytime you touch potentially contaminated surfaces or items.
- Appropriate Use of Personal Protective Equipment (PPE): Your choice of PPE—gloves, gowns, masks, and eye protection—should always be guided by the level of exposure you anticipate. If there's any chance of splashes or sprays, gloves alone aren't enough. Just as crucial is knowing how to put on and, more importantly, take off your PPE without contaminating yourself.
- Safe Injection Practices and Sharps Safety: This is a set of hard-and-fast rules: never recap used needles, dispose of sharps immediately in designated puncture-resistant containers, and always use safety-engineered devices whenever they're available.
- Respiratory Hygiene and Cough Etiquette: This practice extends protection to everyone in the facility. It involves actively coaching patients and visitors to cover their coughs or sneezes and providing them with tissues and hand hygiene supplies to contain the spread of respiratory germs.
By making these principles a consistent, reflexive part of your daily work, you move beyond just following rules. You help build a powerful culture of safety that protects you, your colleagues, and every patient who walks through the door.
Your Essential Toolkit for BBP Safety
Knowing the risks of bloodborne pathogens is only half the battle. The other half is having the right gear and the right habits to keep yourself safe on the job, every single day.
Think of your safety strategy as having two critical layers: the equipment you wear and the environment you control. This is your guide to mastering both your Personal Protective Equipment (PPE) and the essential Engineering and Work Practice Controls that turn safety rules into real-world protection.
Personal Protective Equipment (PPE)
Personal Protective Equipment is your most immediate line of defense. It's the physical barrier you place between yourself and any potentially infectious material.
But just having a box of gloves in the supply closet isn't enough. You have to know precisely what to wear, when to wear it, and—most importantly—how to take it off without contaminating yourself in the process. The specific PPE you need always comes down to the task at hand and the level of exposure you might face.
Here are the core pieces of your PPE arsenal:
- Gloves: This is your most common and fundamental piece of gear. You must wear gloves anytime your hands might come into contact with blood, Other Potentially Infectious Materials (OPIM), or any contaminated item or surface.
- Gowns and Aprons: If there's a chance of splashes or sprays to your body, a gown or apron is a must. Think of procedures like surgery or an autopsy where this risk is high. It's a simple way to protect your skin and clothing.
- Face Masks and Goggles/Face Shields: Your eyes, nose, and mouth are direct pathways for pathogens. These items are non-negotiable whenever splashes, sprays, or droplets of blood or OPIM could be generated.
The most crucial part of using PPE isn't putting it on—it's taking it off. Incorrect doffing procedures can transfer contaminants from the used PPE directly to your skin, defeating the purpose entirely.
Always remove your gear carefully, peeling it away from your body and face. Dispose of it immediately in the designated containers before you even think about leaving the work area. And the final, mandatory step? Thorough hand hygiene right after you take your gloves off.
Designing Safety Into Your Environment
Beyond what you wear, your workplace itself should be engineered to minimize risk from the start. This is where Engineering Controls and Work Practice Controls come into play.
Think of it this way: engineering controls are changes to the physical environment, while work practice controls are changes to your behavior. Together, they build safety directly into your daily routine.
Engineering Controls in Action
These are the smart tools and devices that do some of the safety work for you, removing the hazard at its source.
You're probably familiar with most of them:
- Sharps Disposal Containers: Those classic red, puncture-resistant boxes for used needles, scalpels, and glass. Their entire design is focused on one thing: preventing an accidental stick after a sharp has been used.
- Self-Sheathing Needles: These are a game-changer. They have a built-in safety feature, like a sliding sheath that you activate to cover the needle right after use, dramatically cutting the risk of a needlestick.
- Needleless Systems: Whenever possible, using systems that connect IV lines without a traditional needle eliminates the sharps injury risk from that task completely.
These controls are so effective because they don't depend on someone remembering a safety step in a stressful moment. The safety is built right in. This kind of proactive design is a cornerstone of modern safety, especially in high-pressure fields handled by an emergency response team.
Building Safe Work Habits
Work practice controls are the other side of the coin. These are the conscious, safe habits you develop until they become second nature. They are the human element that makes the whole safety system work.
Key work practice controls you must adopt include:
- Never recapping a used needle: This is a hard and fast rule. Bending, breaking, or recapping a used needle is one of the single most common causes of needlestick injuries. Just don't do it.
- Proper Handwashing: Performing hand hygiene with soap and water or an alcohol-based hand rub is a non-negotiable step after removing gloves and after any potential exposure to blood or OPIM.
- No Eating or Drinking in Work Areas: Keep your food, drinks, makeup, and anything else that might touch your mouth far away from potentially contaminated areas. This simple habit prevents accidental ingestion of dangerous pathogens.
By combining the right PPE for the task with smart environmental controls and rock-solid safe habits, you create multiple layers of protection. This "defense-in-depth" approach is the most reliable way to guarantee your safety and the safety of everyone around you.
What To Do Immediately After An Exposure
Even with the best training and the most careful safety measures, accidents can happen. When they do, the situation is instantly high-stress. In those first few moments, knowing exactly what to do isn't just helpful—it's your most powerful tool for protecting your own health.
The seconds and minutes right after a potential exposure are absolutely critical. What you do next can dramatically reduce your risk of infection. The key is to stay as calm as possible and move through a clear, pre-planned set of actions without hesitation.
Step 1: Immediately Clean The Area
First things first: clean the site of the exposure. The goal is to wash away as much of the potentially infectious material as you can, reducing the viral load right away. How you do this depends on where the exposure happened.
- For skin exposures (like needlesticks, cuts, or bites): Immediately wash the spot with plain soap and water. You don’t need to scrub aggressively or use harsh antiseptics like bleach. In fact, doing so can damage the skin and might even make things worse.
- For mucous membrane exposures (splashes to the eyes, nose, or mouth): Flush the area thoroughly with lots of water or a sterile saline solution. If you wear contact lenses and your eyes were splashed, take them out after an initial flush, then keep rinsing.
This simple act of cleaning is the most important first-aid step you can take. Don't do anything else until you've done this.
Step 2: Report The Incident Promptly
As soon as you've cleaned the area, you need to report what happened. Tell your direct supervisor, the designated safety officer, or whoever your workplace protocol identifies. This isn't a time for embarrassment or second-guessing yourself; reporting is a mandatory step designed to protect you.
Timely reporting is what kicks the entire post-exposure process into gear. It ensures you get the confidential medical attention you need, fast. It also allows your organization to document the event and figure out how to keep it from happening to someone else.
This official report is what unlocks access to confidential medical counseling and treatment, all covered by your employer. The principles of clear, immediate communication are just as vital for keeping your family safe after a potential exposure.
Step 3: Seek A Confidential Medical Evaluation
Once you've reported the incident, you'll be directed to a prompt and confidential medical evaluation, which your employer provides at no cost to you. A healthcare provider will assess your specific situation, determine the level of risk, and lay out the next steps. This will involve documenting the source patient's status (if known) and drawing your blood for baseline testing.
This flowchart shows how the different safety tools—controls, PPE, and practices—work together to prevent these exposures in the first place.
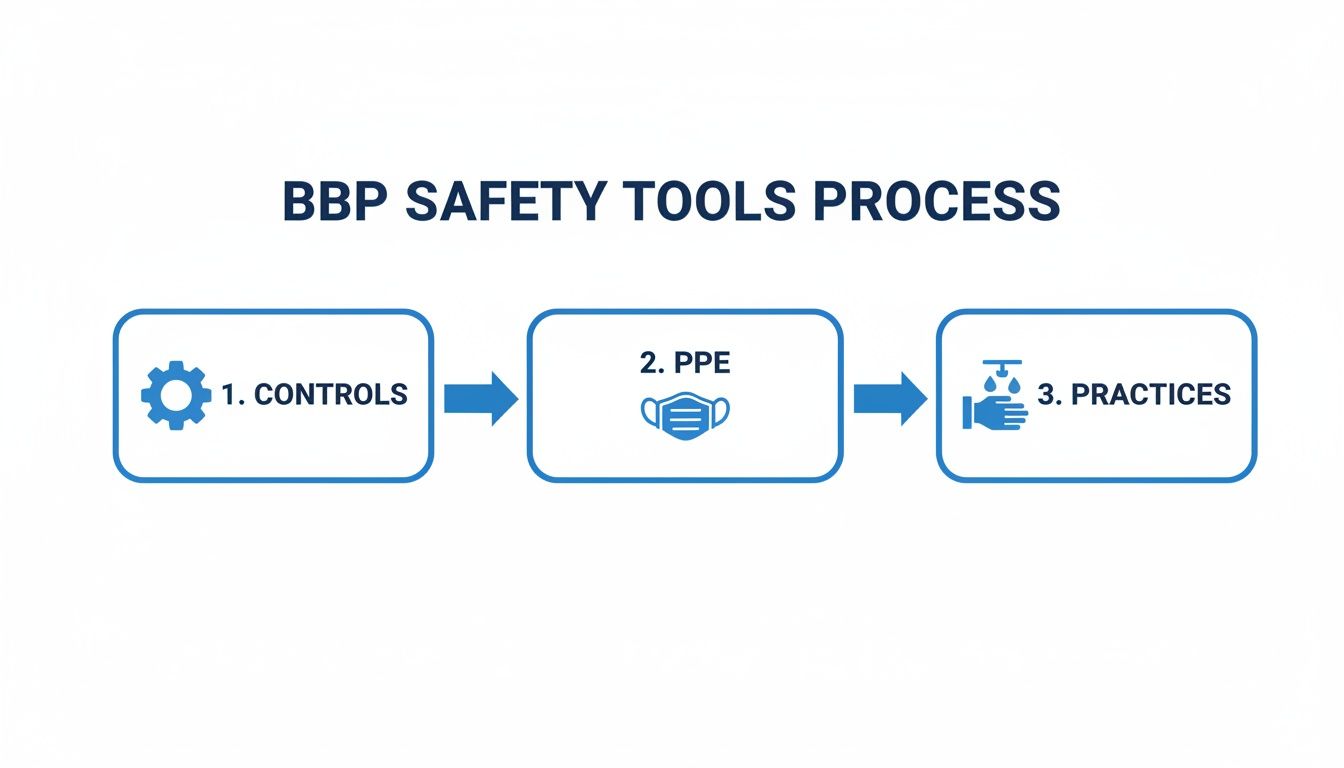
This layered approach is a great reminder of how engineering controls, PPE, and work practices create a solid system to keep you safe.
The most time-sensitive part of your medical evaluation is the conversation about Post-Exposure Prophylaxis (PEP). PEP is a course of antiviral medicine that can stop an infection from taking hold after you've been exposed to a pathogen like HIV or HBV. For PEP to have the best chance of working, it has to be started as soon as possible—ideally within just a few hours of the exposure.
In extreme situations with major biohazard contamination, cleanup may require the help of professional homicide cleanup services to make sure the environment is fully decontaminated. Your own follow-up care will include more testing at set intervals (like 6 weeks, 3 months, and 6 months) to monitor your health.
Why Modern BBP Training Is Moving Online
OSHA's annual bloodborne pathogens training is a non-negotiable part of working in healthcare. But the way you meet that requirement is definitely changing. Rigid, in-person classes are quickly being replaced by flexible, high-quality online education that actually fits a modern professional's schedule.
This isn't just a trend; it's a proven shift. Many peer-reviewed studies and industry articles have shown that well-designed online courses deliver knowledge retention and patient care outcomes that are just as good—and sometimes even better—than sitting in a traditional classroom. Modern, accredited online BBP training provides the same critical information without the logistical headaches.
The Myth of "In-Person Only" Training
For a long time, there was a persistent belief that only courses from big names like the American Heart Association or the American Red Cross were truly "valid." That simply isn’t true anymore. While those organizations absolutely offer quality training, they're no longer the only game in town for accredited certification.
Hospitals, clinics, and major healthcare systems have widely embraced accredited online certifications. They've recognized that a well-built online course delivers standardized, top-tier education with far more convenience. The focus has shifted from how the material is delivered to the quality and accreditation of the curriculum itself.
The core OSHA requirement is that training must be comprehensive and allow for interaction with a qualified instructor. Leading online platforms like ProMed Certifications are built to meet and exceed these standards, giving you the full credibility your employer demands.
The Clear Advantages of Online Certification
Opting for an online BBP course isn't about taking a shortcut; it's a smart, strategic move. Everyone needs thorough training, and learning about effective infection control training for healthcare workers is a key part of that. Online platforms just make it more accessible than ever.
Think about the real-world benefits:
- Unmatched Flexibility: Complete your training when it actually works for you—during a lunch break, late at night, or over a weekend. You’re in total control, which means no more taking time off or traveling to a classroom.
- Self-Paced Learning: Did you get distracted or miss a crucial detail? With an online course, you can rewind and review complex topics as many times as you need. This approach ensures you don't just skim the material on bloodborne pathogens precautions; you master it.
- Cost and Time Savings: Online training cuts out all the extra costs—gas, parking, and lost hours at work. You can get certified efficiently and receive your proof of completion instantly without ever sacrificing quality.
This move to digital learning is happening across all professional development.
At ProMed Certifications, we've been at the forefront of this evolution. We deliver a modern solution that blends convenience with the rock-solid credibility you need to stay compliant and feel confident in your work. Our accredited courses are trusted by thousands of healthcare professionals and institutions for a reason.
Clearing Up Common Questions About BBP Precautions
Even after you’ve got the basics down, some specific questions always seem to pop up when it comes to bloodborne pathogens. It's completely normal. Let's tackle some of the most common ones we hear from healthcare professionals to make sure you feel totally confident in your day-to-day safety practices.
Which Body Fluids Do Standard Precautions Apply To?
This is a big one, and the answer is simple: you apply Standard Precautions to almost everything. The core principle is to treat certain materials as potentially infectious every single time, without exception.
This includes:
- All blood and any products made from blood.
- All body fluids, secretions, and excretions (like saliva, vomit, or urine), except for sweat. This applies whether you can see blood in them or not.
- Non-intact skin, meaning any area with cuts, rashes, or scrapes.
- Mucous membranes—your eyes, nose, and mouth.
Following this approach means you never have to second-guess whether a situation is risky. You just apply the same high level of caution every time, which keeps you safe from both the threats you can see and the ones you can't.
What Is An Exposure Control Plan?
Think of an Exposure Control Plan (ECP) as your workplace’s specific safety playbook for bloodborne pathogens. It’s not just a suggestion; it’s a formal, written document required by OSHA that lays out exactly how your facility eliminates or minimizes your risk of exposure on the job.
An ECP has to cover everything from the proper use of PPE and engineering controls (like sharps disposal containers) to the facility’s free Hepatitis B vaccination program. Most importantly, it details the exact steps to take if an exposure does happen. Your employer is required to review and update this plan annually and must make it available for you to look at whenever you need to.
Is Online BBP Training Valid For OSHA Requirements?
Yes, absolutely. The old belief that only in-person training from certain legacy organizations is legitimate is simply outdated. High-quality online BBP training is a completely valid and widely accepted method for meeting OSHA's annual training requirement.
We're seeing a major shift across the healthcare industry. Hospitals and clinics now widely recognize that accredited online certifications are just as effective—and sometimes even better for knowledge retention, thanks to their flexibility.
The only real requirement is that the course has to be thorough and include a way for you to ask questions of a qualified trainer. All the leading online platforms, including ours at ProMed, have this feature built right in, ensuring we meet and exceed OSHA standards.
Do I Still Need The Hepatitis B Vaccine If I Always Use PPE?
Yes, you do. While PPE is your first line of defense, it’s not infallible. Gloves can get nicked or torn, and even the most seasoned professional can have an accidental needlestick.
The Hepatitis B vaccine isn't a replacement for PPE; it's a completely separate and powerful layer of protection. It gives you long-term, robust immunity against the virus itself. That's why OSHA mandates that employers offer the full vaccine series completely free of charge to any employee with a risk of occupational exposure. It’s a non-negotiable part of a comprehensive safety strategy.
This guide should give you a solid framework for understanding and applying bloodborne pathogens precautions. The key is to turn this knowledge into a consistent daily habit. Staying compliant with your annual training is a critical part of that process.
Ready to get your certifications with a trusted, convenient, and fully accredited provider? ProMed Certifications offers online courses that fit your schedule and are accepted nationwide, backed by our 100% money-back guarantee. Learn more about the courses we offer!
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today