Online Continuing Education Guide for Medical Professionals

A lot of clinicians still hear the same advice: if it wasn’t taught in a classroom, it must be lower quality. That idea is outdated.
Continuing medical education online isn’t a shortcut. It’s a modern delivery model for serious professional learning. When it’s accredited, current, and well designed, it can match in-person education and in many situations fit clinical life better. That matters when your schedule includes rounds, call, charting, family life, and the constant pressure to stay current without losing a day to travel.
The bigger shift is cultural. Hospitals, clinics, and licensing systems increasingly work within a digital education environment. Busy professionals are no longer asking whether online CME is “real.” They’re asking whether it’s accredited, relevant, easy to document, and accepted where they work.
The End of the Classroom-Only Era
The old assumption was simple: real medical education happened in conference halls, hotel ballrooms, and classroom labs. Online learning was treated like the backup option. That’s no longer a useful way to think about professional education.
Accredited CME has grown into a massive system that clearly includes digital delivery as part of routine professional learning. In 2024, accredited CME programs generated a record $3.7 billion in total income, and registration fees made up 55% of that total. In the same reporting, jointly accredited providers delivered 123,175 interprofessional continuing education activities, an 8.1% increase from 2023, which shows how broadly team-based education is being used across healthcare through modern formats.
That scale matters because it tells us something practical. Online CME isn’t a fringe experiment. It’s part of the infrastructure of lifelong learning in healthcare.
Why the old belief keeps lingering
Many clinicians were trained in an era when education and physical presence were tightly linked. If you sat in the room, signed the sheet, and listened to the lecture, the learning felt official. But attendance and educational quality aren’t the same thing.
A strong online course can do things a lecture often can’t:
- Fit clinical reality: You can learn between shifts, after clinic, or over a series of shorter sessions.
- Support review: You can replay, retake, and revisit difficult material instead of hoping you caught it the first time.
- Reduce friction: There’s no travel, no hotel, and no need to block off an entire day for one topic.
- Match how clinicians work: Many healthcare professionals learn best in short bursts tied to immediate patient care problems.
Practical rule: Judge CME by accreditation, relevance, and educational design. Don’t judge it by whether you had to sit in a folding chair to receive it.
What this shift means for working clinicians
If you’re a nurse, physician, pharmacist, or allied health professional, the modern question isn’t “Is online learning legitimate?” It’s “Which online option meets my board, employer, and patient-care needs without wasting time?”
That shift is especially important for professionals who need both continuing education and recurring certifications. For them, the classroom-only mindset creates unnecessary work. Separate registrations, separate portals, separate certificates, separate deadlines. None of that improves care. It just adds administrative drag.
Continuing education should help you stay competent, compliant, and current. It shouldn’t make your life harder.
What Is Continuing Medical Education Online
Continuing medical education online is accredited professional learning delivered through digital platforms instead of requiring you to be physically present in a classroom.
Think of it as a medical learning system you can carry with you. Instead of waiting for a conference date or driving to a training center, you log in from your laptop, tablet, or phone and complete learning activities when they fit your schedule.
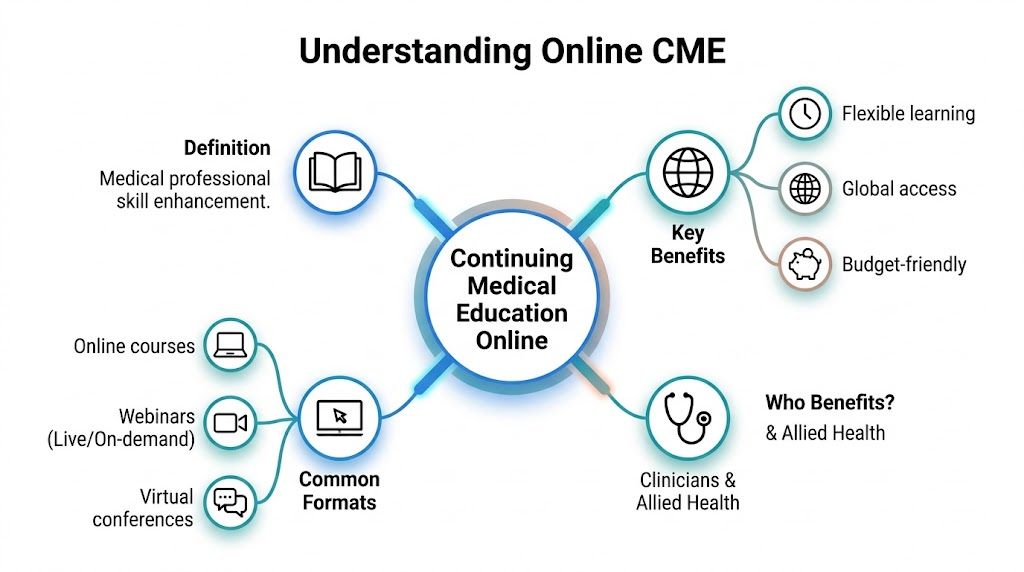
What it actually includes
Online CME is broader than many people realize. It isn’t just recorded lectures.
You may see formats like:
- On-demand courses: Self-paced modules you can start and stop as needed
- Live webinars: Scheduled online sessions with faculty and audience interaction
- Case-based learning: Clinical scenarios that ask you to apply judgment, not just recall facts
- Article-based activities: Read, reflect, and complete a post-test or evaluation
- Podcast or audio learning: Useful during commutes or between tasks when offered for credit
- Virtual conferences: Multi-session events delivered online instead of in person
- Mobile learning: Activities designed to work on a phone, often in short segments
Some clinicians expect online CME to feel passive. In reality, the better programs are structured around decisions, reflection, feedback, and practical application.
Why healthcare professionals use it
Individuals often first encounter online CME because they need to maintain licensure, board status, or employer compliance. That’s valid, but it’s only part of the picture.
Online CME also helps you:

This is one reason digital learning works so well for experienced clinicians. Adult learners usually want education they can use right away. They don’t want filler. They want clear takeaways that connect to the next patient, the next shift, or the next renewal deadline.
What confuses people most
The word “online” often gets mixed up with “informal.” Those aren’t the same thing.
An accredited online CME activity still has structure. It typically includes a learning objective, faculty or editorial oversight, credit designation, a completion process, and a certificate. The platform may feel more flexible, but the activity still has to meet educational standards.
Online CME is not “random medical content on the internet.” It’s organized, credit-bearing education delivered through a different channel.
Where certifications fit in
Many guides stop too early. They explain online CME, then ignore the reality that many professionals also need certifications such as ACLS, PALS, BLS, CPR, or neonatal resuscitation pathways depending on role and workplace expectations.
That creates a practical question: should your continuing education and certification needs live in separate systems, or can they be managed together? For many clinicians, that’s the difference between a manageable renewal cycle and a scattered one.
The Truth About Accreditation and Industry Acceptance
The most persistent myth in this space is that only a legacy classroom provider counts. You still hear versions of it in break rooms and orientation packets: if it’s not from a familiar in-person brand, it won’t be accepted.
That belief confuses brand recognition with accreditation.
When boards, employers, and compliance teams review education, they usually care about whether the activity is accredited, whether the credits match the requirement, and whether the documentation is complete. The provider’s logo matters far less than clinicians often assume.

What accreditation tells you
Accreditation is the quality signal that matters. It tells you the education has been reviewed within a recognized standards framework.
For clinicians, that usually means asking questions like these:
- Who accredits the activity? Look for the accrediting body relevant to your profession.
- What credit type is offered? The credit has to match your license or board requirement.
- Is the documentation usable? Your certificate should clearly identify the activity and awarded credit.
- Is the content current? Accreditation matters, but outdated content is still a problem.
Why online learning can be equal or stronger
A well-built online activity isn’t merely a recorded lecture posted on a website. Good digital instruction uses design choices that help clinicians retain and apply information.
One example is microlearning. Modern online learning uses shorter, focused modules that reduce overload and support review. In the evidence summarized in this peer-reviewed article on digital health professions education, microlearning improved knowledge retention by 17% to 20% at 3-month follow-up, compared with 10% for traditional lectures.
That doesn’t mean every online course is automatically good. It means the format itself can support strong outcomes when it is designed well.
Don’t ask whether online learning is “less real.” Ask whether the course is accredited, updated, and built for actual learning instead of passive viewing.
Why familiar names still dominate the conversation
People trust what they already know. That’s understandable in healthcare, where risk matters. But familiarity can also freeze decision-making.
A hospital educator may keep defaulting to the same in-person vendors because they’ve used them for years. A clinician may assume a national brand is the only safe choice because nobody ever explained the underlying accreditation logic. Once you understand that logic, the market looks very different.
You can also see this shift in how digital education is built. Many organizations now use learning standards that make courses trackable, portable, and easier to manage across systems. If you’re curious how course developers structure that behind the scenes, this overview of tools to create SCORM compliant courses helps explain why some online platforms feel smooth while others feel clunky.
Hands-on skills and online coursework are not opposites
Some hesitation comes from a reasonable concern: medicine is physical work. People intubate, compress, defibrillate, assess, communicate, and intervene. So how can online education be enough?
The answer is that different learning goals need different delivery methods. Knowledge review, pharmacology, rhythm interpretation, case analysis, guideline updates, and cognitive decision pathways work very well online. Skill validation may be separate depending on the credential, employer, and role. That doesn’t make the online portion less valid. It means the education is being matched to the task.
The strongest mindset is simple: use online education for what digital learning does well, and use in-person skill checks when a specific requirement calls for them. That’s not a compromise. It’s good educational design.
How to Complete and Document Your Online CME
Many clinicians delay CME because the process feels harder than it is. In practice, it’s usually a sequence of small decisions. Once you know the order, it becomes manageable.

Start with your actual requirement
Before choosing a course, confirm what you need for your state, specialty, employer, or certification cycle. The requirement may involve a total number of credits, a particular topic, or a specific type of credit.
Write down:
- Your deadline
- Your required credit type
- Any mandatory topics
- Whether reporting is automatic or self-reported
That short list prevents a common mistake. Clinicians often complete useful education that doesn’t satisfy the technical requirement they were trying to meet.
Choose a provider that makes documentation easy
A provider should make it obvious what you’re earning, how completion works, and where your certificate will appear. If you have to dig through vague menus to figure that out, expect the rest of the process to be frustrating too.
Look for:
- Clear credit labeling: You should know exactly what type of credit the course awards.
- Visible completion steps: Post-tests, evaluations, and certificate release should be explained upfront.
- Downloadable records: You want easy access to certificates if an employer or board asks later.
- Reporting support: If your state uses reporting systems, the provider should explain how that works.
For nurses and other professionals who report through CE Broker, understanding the reporting side matters as much as course completion. This walkthrough on managing a CE Broker account helps clarify what gets tracked and what you may still need to verify yourself.
Move through the activity with intention
Online CME works best when you treat it as applied learning, not background noise. Don’t click through a module while answering messages and expect the material to stick.
A simple approach helps:
- Read the learning objectives first
- Identify one problem from your practice that connects to the topic
- Take brief notes on anything you’d change tomorrow
- Complete the assessment while the material is fresh
- Save the certificate immediately
A certificate is the final administrative step. The real value is whether the course changes a clinical decision, improves a handoff, or sharpens a treatment plan.
A practical example of point-of-care learning
One of the most useful online CME formats is internet point-of-care learning. This turns part of your everyday clinical work into a structured credit activity instead of asking you to carve out separate classroom time.
According to the University of Washington Health Sciences CME guide, physicians can earn 0.5 AMA PRA Category 1 Credits™ per documented cycle by doing three things:
- Identifying a clinical question from practice
- Searching an accredited resource for an answer
- Documenting the question, source, and how the information applies to patient care
That model is useful because it mirrors how clinicians already think. A patient raises a management question. You verify the evidence in an accredited resource. You apply it. Then you document the learning.
Keep your records tidy
You don’t need an elaborate tracking system, but you do need a reliable one. Store certificates in a dedicated folder, keep a running list of completed activities, and save confirmation emails until your reporting cycle closes.
If your platform offers automatic reporting, that can reduce paperwork. Still, it’s smart to verify that the activity posted correctly. Automation helps, but your license is still your responsibility.
A simple personal log can include:

That small habit saves a lot of stress at renewal time.
How to Evaluate Online CME Providers
Choosing a provider isn’t just about price or course count. You’re trusting a platform with your time, your compliance record, and often your renewal deadline. A good provider makes that easy. A weak one creates uncertainty at every step.
A practical checklist
Use this checklist before you enroll.
- Accreditation first: Confirm the provider clearly states who accredits the activities and what credit type is offered.
- Relevant library: Look for topics that match your role, not just a long catalog with little clinical depth.
- Usable platform: The site should work well on mobile and desktop, especially if you learn between shifts.
- Straightforward certificates: You should know where records live and how quickly they appear after completion.
- Support access: When reporting or login issues happen, responsive support matters.
- Clear policies: Refunds, expiration rules, retakes, and employer acceptance details should be easy to find.
Signs a provider may create problems
Some warning signs show up quickly.
A provider may not be the right fit if it:
- Hides accreditation details
- Uses vague language about acceptance
- Makes you contact support just to understand credit eligibility
- Offers a dated interface that’s challenging to use on a phone
- Provides little information about accessibility needs
Accessibility deserves more attention than it usually gets. If a platform uses poor contrast, confusing navigation, or media that doesn’t adapt well to assistive tools, it creates barriers for clinicians.
Compare the experience, not just the catalog
A provider with a smaller but well-organized library may be more useful than one with a huge catalog and poor filtering. The same goes for assessment design. Short, clear quizzes and immediate certificate access often matter more than flashy marketing.
Here’s a quick comparison framework:

The easiest provider to buy from isn’t always the easiest provider to live with during a renewal cycle.
Ask one final question
Does this platform reduce administrative work, or add to it?
That question often reveals the right choice. If the answer is unclear, keep looking.
The ProMed Advantage Bundling CME and Certifications
One of the least discussed frustrations in professional education is fragmentation. A clinician may use one portal for CME, another for ACLS renewal, a different site for BLS, and a separate reporting system for records. That setup is common, but it isn’t efficient.
The demand for a bundled model is real. A 2023 survey found that 68% of physicians want integrated recertification pathways that combine CME with certifications to reduce administrative burden, as summarized in this Pri-Med referenced discussion. The same material notes that relatively few online platforms offer that combined approach with features such as unlimited retakes and guaranteed acceptance.
Why bundling matters in real life
For clinicians, bundled education solves everyday problems:
- Fewer accounts to manage: One login is easier than several.
- Less deadline confusion: Your required learning lives in one system instead of scattered reminders.
- Cleaner records: Certificates and course history are easier to locate.
- Smoother renewals: You spend less time reconstructing what you already completed.
This matters most for professionals whose compliance burden is mixed. A nurse may need continuing education, pharmacology content, and life-support renewals. A physician may need board-relevant CME, DEA-related content, and certification updates. Separate systems can handle those needs, but they often do it awkwardly.
What an integrated option should include
If you’re looking at a bundled model, evaluate it on practical features rather than sales language.
A strong option should offer:

One example is ProMed Certifications, which offers online certification pathways alongside accredited continuing education options, with features such as self-paced access, unlimited retakes, digital certificates, and employer acceptance policies described on its site. For clinicians who want a single system rather than several, that integrated structure can be easier to manage.
The broader takeaway
Bundling isn’t just about convenience. It reflects a better understanding of how healthcare professionals maintain competence. In real practice, continuing education and recurring certification aren’t separate parts of life. They overlap constantly.
When a platform combines them well, you spend less energy on logistics and more on learning that supports patient care.
Frequently Asked Questions About Online CME
Will my employer or board really accept online CME
Usually, the key issue is whether the activity is properly accredited and documented for your profession. Many clinicians worry about the delivery method first, but acceptance decisions usually focus on credit type, accrediting framework, and whether the activity meets the stated requirement.
If you’re unsure, check your board language and your employer’s policy. Look for specifics. “Online” by itself usually isn’t the deciding factor.
Is online learning really as effective as a live lecture
It can be. In many cases, it’s better suited to how working clinicians learn.
The strongest online courses let you pause, review, repeat, and apply content at your own pace. That’s especially helpful when you’re studying complex material after a long shift. A lecture gives you one pass. A digital course can give you structured repetition.
If learning has to fit around patient care, flexibility isn’t a luxury. It’s part of what makes the education usable.
How can online education help with hands-on certifications
Online learning is excellent for cognitive preparation. It can reinforce algorithms, medication review, rhythm recognition, team roles, and sequence-based decision-making. If a specific credential or employer requires separate skill validation, the online portion still has value because it prepares you for that hands-on component efficiently.
That’s why it helps to stop treating online and in-person formats like rivals. They can work together.
Does online CME feel too isolated
Not necessarily. Many online activities include interactive cases, reflection prompts, post-tests, downloadable resources, and live virtual options. Some clinicians engage more thoroughly online because they can focus without travel fatigue, crowded schedules, or the pressure of a packed conference day.
The better question is whether the activity asks you to think, decide, and apply. If it does, it’s not passive.
What if I work in an area with weak internet
That concern is real. According to the discussion referencing WHO data, 40% of global health workers reported connectivity barriers in 2025. That’s a major reason to look for low-bandwidth design, mobile-friendly access, and platforms that avoid making every activity dependent on heavy streaming.
If your connection is unreliable, check a provider’s technical requirements before enrolling. Simpler interfaces, downloadable materials, and mobile access can make a real difference.
Do I need to choose between convenience and quality
No. That’s one of the most outdated assumptions in healthcare education.
Convenience doesn’t mean low standards. It means the learning is designed around clinical work. Quality still comes from accreditation, current content, sound instructional design, and reliable documentation.
If you’re ready to simplify renewals and keep your education in one place, ProMed Certifications offers online certifications and accredited continuing education built for busy healthcare professionals who need flexible, documented, self-paced learning.
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today