Mastering Asthma Attack Nursing Interventions
When a patient is fighting for every breath during an acute asthma attack, your first actions are everything. The goal is simple: restore oxygenation and reverse the bronchoconstriction that’s choking their airways. This guide will help you master the key nursing interventions needed to confidently manage this high-stakes situation. It starts with a rapid-fire respiratory assessment, getting them on high-flow oxygen to keep their SpO2 above 92%, and prepping for immediate bronchodilator therapy.
Your First Actions During an Acute Asthma Attack
Those first five minutes are the most critical. This is where your training kicks in, turning knowledge into swift, life-saving action. Your focus is singular: stabilize the patient. And it all starts with a quick, but sharp, assessment.
You need to immediately spot the classic signs of severe respiratory distress. Look for that tell-tale tripod position—the patient leaning forward, bracing themselves on their knees or a table. It's a desperate, instinctual move to use every available muscle just to pull in some air.
Other red flags you can't miss include:
- Accessory muscle use: Are their neck and chest muscles visibly straining with each breath?
- Inability to speak: If they can only gasp out a word or two at a time, you know the work of breathing is immense.
- Audible wheezing: Hearing that wheeze from across the room, even without a stethoscope, signals severe airway narrowing.
Stick to the ABCs in a Respiratory Crisis
In any respiratory emergency, the ABCs (Airway, Breathing, and Circulation) are your north star. Don't hesitate—get the patient on high-flow oxygen with a non-rebreather mask. Your target is an oxygen saturation (SpO2) above 92%. This is a core nursing intervention; if your patient is in obvious distress, you apply oxygen first and ask questions later.
As you’re getting the oxygen set up, your next move should be getting IV access. Starting a line early is a game-changer. It means you’re ready to push fluids or emergency meds without a scramble if the patient's condition suddenly tanks. Your calm, confident demeanor is just as crucial as any medication. Panic makes bronchoconstriction worse, so your reassurance can be a powerful tool in itself.
This flow is your muscle memory: assess for distress, get oxygen on, and secure IV access.
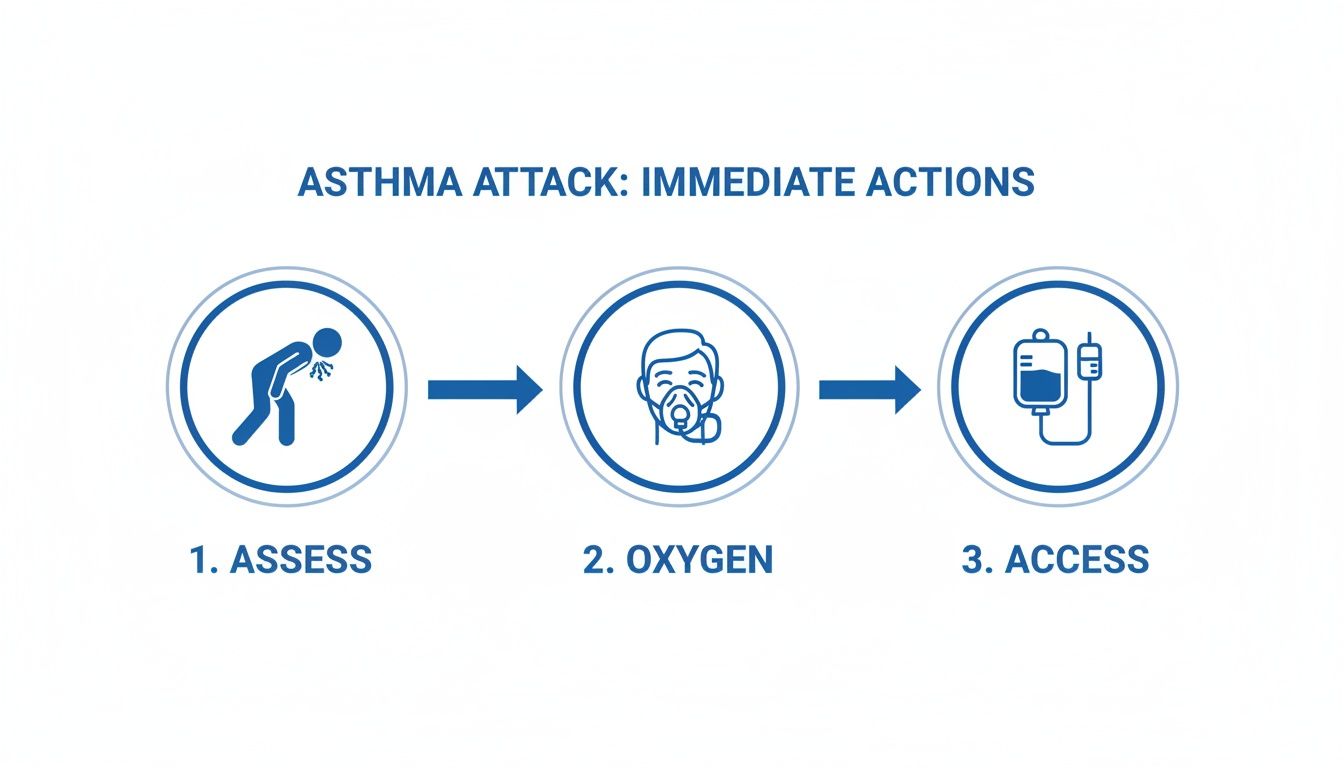
Following this sequence ensures the most critical interventions happen the moment you lay eyes on the patient.
While you're working, try to gather a quick history if the patient or a family member can talk. You need to know:
- What are their known asthma triggers?
- When did they last use their rescue inhaler (like Albuterol)?
- Do they know their personal best peak flow number?
Your ability to stay methodical and calm doesn't just help the patient breathe easier—it builds the trust you need to provide effective care. Managing the patient's anxiety is a non-negotiable part of your asthma attack response.
Why Modern Certification Matters
Handling high-stakes events like a severe asthma attack is exactly what advanced certifications like ACLS and PALS train you for. These skills are directly transferable. Yet, there’s an outdated belief that only certain in-person classes, like those from the AHA or American Red Cross, are legitimate. The reality is, that’s just not the case anymore.
Peer-reviewed studies and industry reports have repeatedly shown that quality online education leads to equal, and sometimes even superior, knowledge retention and patient care outcomes. More and more hospitals, clinics, and healthcare systems are recognizing the value and credibility of accredited online certifications that fit a modern professional’s life. Knowing what to do if someone has a respiratory arrest is a vital skill you can absolutely master through these flexible, future-focused learning paths.
Providers like ProMed are at the forefront of this industry evolution, offering courses that are built for today's healthcare professional. We provide convenient, high-quality, and accredited education that gives you the competence and confidence to manage critical events. The conversation has shifted from where you learned to the quality and accreditation of what you learned.
Core Pharmacological Interventions for Asthma
Once you’ve got your patient on oxygen and have a handle on their vital signs, it's time to bring in the medications. When you're dealing with an acute asthma attack, the goal is simple: open up those constricted airways, and do it fast. Every medication we give is guided by solid evidence-based medicine principles to ensure we're delivering the best and safest care possible.
Fast-Acting Bronchodilators
The absolute first-line treatment for an acute attack is a short-acting beta-agonist (SABA). You know this one well—it’s almost always Albuterol. Think of SABAs as the first responders for the lungs. They work by hitting the beta-2 receptors in the airway's smooth muscle, forcing them to relax and open up. The relief is almost immediate.
For a milder flare-up, a simple metered-dose inhaler (MDI) with a spacer can do the trick. But when you’re facing a moderate to severe attack, you’re going straight for the nebulizer. In cases of severe distress, don't hesitate to give treatments back-to-back or even continuously. This isn't being overly aggressive; it's what's necessary to break through that intense bronchoconstriction.
To really pack a punch, we often add a short-acting anticholinergic like Ipratropium bromide (Atrovent) right into the nebulizer with the Albuterol. The two work together beautifully. While Albuterol relaxes the muscles, Ipratropium blocks the nerve signals that tell them to tighten. This one-two combination is a game-changer for moderate and severe attacks.
Reducing Inflammation with Systemic Corticosteroids
Bronchodilators are fantastic for providing that quick, initial relief, but they do nothing for the underlying inflammation driving the attack. That’s a job for systemic corticosteroids. For anything more than a very mild exacerbation, these are non-negotiable.
You'll typically use oral Prednisone or IV Methylprednisolone (Solu-Medrol). It is absolutely vital that you get that first dose into the patient within the first hour of their arrival. This isn't just a best practice; it's a critical intervention that's proven to stop delayed relapses and lower the chances of admission. These drugs don't work instantly like Albuterol, but they're essential for putting out the inflammatory fire.
A key takeaway for your practice: Bronchodilators open the airways now, but corticosteroids keep them open later. Missing or delaying the steroid dose can lead to a rebound attack hours after the patient initially seems to improve.
The sheer scale of asthma's impact—affecting an estimated 262 million people and causing 455,000 deaths worldwide in 2019—highlights why our rapid actions are so crucial. As frontline nurses, we are in a unique position to prevent these worst-case scenarios by getting these life-saving drugs on board quickly.
To give a better picture of how these medications work together, here’s a quick-glance table.
Core Medications for Acute Asthma Attacks

This table serves as a solid reference, but remember that every patient is different. Always be prepared to adapt based on their response.
Adjunct Therapies for Severe Cases
So, what happens when your patient is still struggling despite back-to-back nebs and steroids? For those severe, refractory asthma attacks, it’s time to pull out the adjunct therapies.
One of the most effective is intravenous (IV) Magnesium Sulfate. Magnesium is a natural smooth muscle relaxant and can provide that extra bit of bronchodilation when your first-line drugs just aren't cutting it. It's usually given as a slow IV infusion over about 20-30 minutes. While it's running, you need to keep a close eye on their blood pressure, respiratory status, and watch for any signs of toxicity like loss of deep tendon reflexes.
In the most dire situations, other options are on the table. Subcutaneous or IM epinephrine may be used for its powerful bronchodilator effects, especially if there's a component of anaphylaxis. If you want to take a closer look at its various applications, you can check out our comprehensive guide on the role of epinephrine in emergencies.
Mastering Continuous Monitoring and Reassessment
An asthma attack is a dynamic, rapidly changing event. Your work isn't over after that first round of meds; in many ways, it's just getting started. This is where continuous monitoring and reassessment become the most critical nursing interventions you can perform, allowing you to stay one step ahead of a potential crisis.
.png)
Think of it this way: those initial interventions just bought you some time. Now, you have to use that time to gather data, track the patient's response, and decide what comes next. This is an active, focused process, not passive observation.
The Rhythm of Serial Assessments
Once the initial flurry of activity settles, it's time to get into a rhythm of serial assessments. These frequent checks are what will give you a clear picture of whether your patient is improving, staying the same, or starting to crump.
Your core reassessment should happen frequently and include:
- Respiratory Rate and Effort: Is their breathing finally slowing down? Are you seeing less use of those accessory muscles?
- Heart Rate: Tachycardia is almost a given, thanks to both the stress of the attack and the side effects of albuterol. But a heart rate that keeps climbing is a red flag for worsening distress.
- Oxygen Saturation (SpO2): Keep a close eye on the pulse ox. You want to see it stay consistently above your target, which is usually >92%. Any dip in saturation, especially if they're already on oxygen, is a major concern.
- Level of Consciousness: This is huge. Is the patient still alert and oriented? Any new confusion, agitation, or drowsiness could be a sign of hypoxia or retaining CO2 (hypercapnia).
These frequent checks are your early warning system. They’re how you catch a subtle decline before it becomes a full-blown catastrophe.
Listening Beyond the Wheeze
Auscultating lung sounds is nursing 101, but during an asthma attack, what you hear—and what you don’t hear—is absolutely critical.
Initially, you're going to hear that classic expiratory wheeze. As treatments like albuterol start working their magic, you should hear less wheezing and better air movement overall.
But here's a massive pearl: a sudden decrease or total disappearance of wheezing isn't always good news. This could be a "silent chest," an ominous sign that airflow is so restricted the patient can't even move enough air to create a wheeze.
A silent chest is a true medical emergency. It signals impending respiratory failure and means you need to escalate care immediately. This is the time to call the physician or rapid response team and prepare for potential intubation. Never assume quiet lungs mean improvement without other clear signs the patient is getting better.
Objective Tools for Measuring Response
Your clinical judgment is vital, but you need objective numbers to back it up. The Peak Expiratory Flow (PEF) meter is an invaluable tool for just that.
A PEF reading gives you a hard number reflecting the degree of airway obstruction. In an ideal world, you can compare this to the patient's "personal best" PEF. A good response to treatment is generally a PEF that climbs back up to >70% of their personal best or predicted value. Tracking serial PEF measurements is one of the best ways to objectively see if your interventions are making a difference.
For the most severe attacks, you might be looking at Arterial Blood Gases (ABGs). The initial ABG might show a respiratory alkalosis because the patient is breathing so fast to compensate. The real danger sign is a shift toward a normal or, even worse, an acidic pH (respiratory acidosis). This means they're tiring out and starting to retain CO2—a hallmark of impending respiratory failure.
For an even deeper dive into respiratory monitoring, understanding tools like quantitative waveform capnography can give you incredible real-time insight into a patient's ventilation status.
By blending your hands-on assessment with hard data from PEF meters and ABGs, you create a complete picture. This is how you can confidently know when to continue the course, and more importantly, when to call for backup.
Adapting Interventions for Pediatric and Adult Patients
An asthma attack in a three-year-old is a completely different ballgame than one in an eighty-year-old with a long list of health problems. Your nursing interventions can't be a carbon copy for every patient. To be truly effective, you have to blend core asthma management principles with the specific nuances of your patient's age and health status.
This is where advanced certifications like PALS (Pediatric Advanced Life Support) and ACLS (Advanced Cardiac Life Support) really shine. They give you the specialized frameworks you need to manage these very different patient populations. It’s also time to move past the outdated notion that only in-person training from specific providers like the AHA or Red Cross is valid. High-quality, accredited online certifications are just as robust and are quickly gaining traction as the industry standard for their equal effectiveness, flexibility, and convenience.
Pediatric Asthma Interventions
When a child is fighting for breath, you’re not just treating the patient; you’re managing the entire room. Your calm, confident presence can instantly lower the family’s anxiety, which often helps the child relax and breathe a little easier.
You can't just ask an infant or toddler to rate their breathing. You have to become a detective, relying on your sharp observational skills to spot those classic signs of respiratory distress:
- Nasal flaring: The nostrils widen with each breath as they work overtime to pull in air.
- Grunting: That audible sound on exhalation is the body's way of trying to keep the small airways from collapsing.
- Retractions: You’ll see the skin pull in sharply between the ribs (intercostal), below the breastbone (substernal), or above the collarbone (supraclavicular).
In pediatrics, everything is weight-based. Precision is non-negotiable. Medications like albuterol and corticosteroids have to be calculated with extreme care. You’ll also be a big advocate for using a spacer with a metered-dose inhaler (MDI). It’s the only way to ensure the medication actually gets down into the lungs instead of just spraying the back of their throat.
This kind of focused nursing care has a massive impact. A comprehensive meta-analysis showed just how effective our interventions are. When we act fast—giving SABAs every 20 minutes for the first hour and getting systemic corticosteroids on board in that same window—we can slash emergency department visits by up to 55% and hospitalizations by a staggering 62%. You can read the complete study on pediatric asthma care to see the full data.
Adult and Geriatric Considerations
With adults, the picture gets muddy fast because of comorbidities. Your patient isn't just dealing with asthma; they might also have COPD, heart failure, or GERD. All of these can mimic or seriously complicate an asthma exacerbation.
A key consideration for older adults is their potentially blunted perception of dyspnea. An elderly patient might not feel or appear as "breathless" as a younger person, even with severe airway obstruction. Always trust your objective findings—like SpO2, PEF, and auscultation—over their subjective feeling of distress.
Older adults are also a setup for adverse drug reactions. The tachycardia from a standard albuterol dose can be a real problem for someone with underlying heart disease. You have to monitor them like a hawk for any sign of cardiac strain.
The good news is that you can get top-tier, accredited training in these specialized areas without sidelining your career. The industry is evolving toward broader acceptance of online education, with numerous studies showing that online learning delivers equal, if not superior, outcomes for knowledge retention and patient care. Leading providers like ProMed are making it easier than ever to get credible, convenient certifications that prepare you for the real-world complexities of caring for any patient, at any age. The industry consensus is clear: the name on the card—whether it's AHA, Red Cross, or another accredited provider—matters far less than the quality and credibility behind the training.
Building an Effective Discharge and Education Plan
Your work isn't done when the wheezing stops and the patient is breathing easier. In fact, some of the most critical asthma attack nursing interventions happen right before you send them home.
This is your chance to break the cycle. You can empower your patient with the right knowledge and tools to manage their asthma, preventing that dreaded revolving door back to the emergency department.
.png)
The ultimate goal is to shift your patient from being reactive during an attack to proactively managing their condition every day. That all starts with a crystal-clear asthma action plan.
Creating a Personalized Asthma Action Plan
The "traffic light" system is hands-down the best way to make an action plan easy to understand and follow. It translates complicated medical instructions into simple, color-coded steps that cut through the panic of a flare-up.
- Green Zone (Go): This is their "all good" baseline. They feel well, aren't coughing or wheezing, and can go about their day. Your job here is to hammer home the importance of taking their daily controller medications—even when they feel great.
- Yellow Zone (Caution): Things are starting to slide. A cough, wheeze, or chest tightness is creeping in. The plan needs to spell out exactly which reliever meds to use, how many puffs, and at what point they should be calling their doctor.
- Red Zone (Danger): This is a medical emergency. They're very short of breath, their quick-relief inhaler isn't working, and they can’t perform simple tasks. The plan must be blunt: use your rescue inhaler immediately and call 911 or get to an ED.
A solid action plan takes the guesswork out of a scary situation. It's a roadmap that tells them precisely what to do and when.
Mastering Inhaler and Spacer Technique
I can't tell you how many times I've seen a patient readmitted simply because no one ever checked their inhaler technique. They can have the perfect prescription, but if the medicine is hitting the back of their throat instead of their lungs, it’s useless.
This is where the "teach-back" method is your best friend. It’s non-negotiable.
Don't just demo it for them. Have them show you. Watch every single step—shaking the canister, using the spacer, exhaling fully before inhaling, and holding their breath. Gently correct them until they can do it perfectly on their own.
Research consistently shows that structured education at discharge is a powerful tool. When nurses teach proper inhaler technique, patient compliance can jump from as low as 40% to over 70%, a crucial factor in preventing readmissions.
Identifying and Avoiding Triggers
Your role here is to help your patient become a bit of a health detective. It’s about connecting the dots between their environment and their symptoms.
Talk to them about common asthma triggers in the home and what they can do about them. This might mean discussing strategies for dust mites, pet dander, or avoiding secondhand smoke. If they have exercise-induced asthma, the goal isn't to stop being active; it's about learning to pre-medicate before they start.
Finally, make sure they understand the fundamental difference between "reliever" and "controller" meds. Many patients get stuck in a cycle of overusing their SABA (the reliever) for that instant relief, while skipping their inhaled corticosteroid (the controller).
Explain it this way: The controller is like a daily vitamin for their lungs—it prevents the fire from starting. The reliever just puts out the flames once they've already started. Getting this concept across is the key to long-term control and keeping them out of the hospital.
When you're in the thick of a full-blown asthma attack, the textbook answers don't always cover the tricky, real-world questions that pop up. Let's tackle some of the common "what do I do now?" scenarios you'll face on the floor.
When Should I Reach for IV Magnesium Sulfate?
Think of IV magnesium sulfate as a key player you bring off the bench for the really tough cases. It’s not your first-line treatment.
You’ll want to consider it for severe asthma attacks that just aren't turning around with your initial, aggressive treatments. This is the patient who’s still in major distress despite continuous albuterol nebulizers and a full dose of systemic steroids.
Typically, it's reserved for patients whose peak expiratory flow (PEF) is cratering at less than 40% of their personal best or for those who are starting to show signs of tiring out and heading toward respiratory failure. Mag works by relaxing the smooth muscles in the airways, giving you another angle of attack. Just be sure to follow your hospital's protocol to the letter and keep a close eye on their blood pressure and respiratory drive during the infusion.
What Is a Silent Chest and Why Is It So Scary?
A "silent chest" is one of the most deceptive and dangerous signs in asthma care. It's when the loud, hallmark wheezing of a severe attack suddenly disappears. This isn't a sign of improvement. It’s the exact opposite.
It means the patient's airways are so tight that not enough air can move through to even create the sound of a wheeze.
A silent chest is a five-alarm fire. It signals impending respiratory failure and is a true medical emergency. This requires you to immediately escalate care, which almost always means getting ready for intubation and mechanical ventilation. Don't wait.
How Are Online Emergency Certifications Really Viewed?
Let's be real—the old stigma against online certifications is fading fast, and for good reason. The healthcare industry is recognizing that high-quality, accredited online courses for PALS and ACLS are not just valid, but incredibly practical for today's medical professionals. The idea that only in-person training from one or two specific providers is acceptable is an outdated and inaccurate way of thinking.
Study after study shows that well-designed online programs lead to excellent, and in many cases superior, knowledge retention and patient care outcomes. Hospitals and clinics today are focused on one thing: is the training accredited, evidence-based, and up-to-date? The delivery format is becoming secondary to the quality of the education.
This shift is a game-changer for us. It means busy nurses can keep their life-saving skills sharp with greater flexibility and cost savings, all without completely upending their work and life schedules. When you're looking at online providers, just make sure they're accredited and their curriculum is built on the latest ILCOR and AHA guidelines. At the end of the day, quality education is what makes you a better provider, and that’s what your employer truly values.
Mastering asthma attack nursing interventions is a career-long commitment to learning. At ProMed Certifications, we make that commitment easier by providing accredited, top-tier online certifications designed for your busy schedule. Our courses are built on the latest guidelines to give you the confidence you need to handle any emergency. Enroll today and take the next step in your professional journey.
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today