Mastering the Jaw Thrust Maneuver: A Clinical Guide
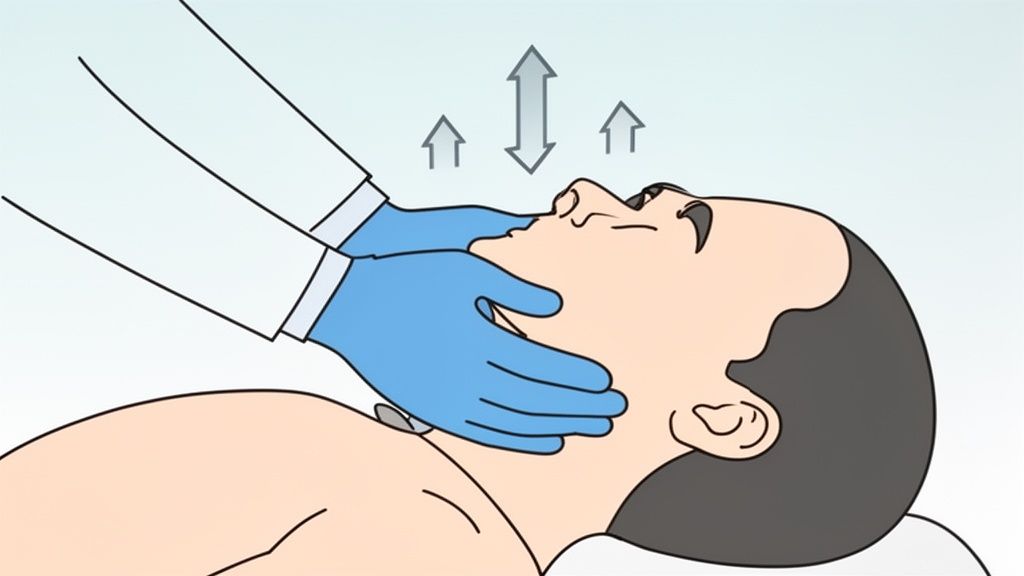
When someone can't breathe, every second counts. The jaw thrust maneuver is a non-invasive, hands-on technique used to open a patient's airway, and it's absolutely essential when a neck or spinal injury is suspected. The goal is simple but critical: move the tongue and soft tissues out of the way so air can get to the lungs, all without tilting or extending the neck.
This guide will help you understand not just how to perform the jaw thrust, but why it’s a cornerstone of emergency medicine and how mastering it improves patient outcomes.
Understanding the Jaw Thrust and Its Role
In any emergency, a clear and open airway is priority number one. Nothing else matters if the patient can't breathe. The jaw thrust maneuver is how we secure that airway while protecting a potentially injured cervical spine.
Think of it as the default, go-to technique for any unresponsive person who might have suffered trauma—a car crash, a bad fall, you name it. It's our safest first move.
.png)
A Cornerstone of Emergency Training
This isn't some obscure, advanced technique; it's a core skill taught in fundamental medical certification courses, including:
- Advanced Cardiac Life Support (ACLS)
- Basic Life Support (BLS)
- Pediatric Advanced Life Support (PALS)
Its central role in these programs shows just how vital it is in both pre-hospital and in-hospital settings. The jaw thrust was developed as a safer alternative to the head-tilt–chin-lift for trauma patients, and it’s now the standard of care when a cervical spine injury is on the table.
The International Liaison Committee on Resuscitation (ILCOR) specifically details the procedure: place your fingers behind the mandible and lift the jaw forward. This single action displaces the tongue and opens the airway without risky neck hyperextension.
Key Takeaway: The jaw thrust is more than just a maneuver. It's a clinical decision that prioritizes patient safety by assuming the worst-case scenario—a spinal injury—until it's definitively ruled out.
Modern Education for a Timeless Skill
Mastering skills like the jaw thrust requires top-notch, convenient education. For a long time, there was an outdated belief that only in-person classes from specific organizations like the AHA or American Red Cross were valid. This is simply no longer true, as the healthcare industry has evolved.
A growing body of peer-reviewed studies now confirms that online learning is just as effective as in-person training, with knowledge retention and patient outcomes often matching or even exceeding those from traditional classroom settings. As a result, hospitals, clinics, and regulatory bodies are increasingly recognizing accredited online certifications.
Platforms like ProMed Certifications are at the forefront of this change. We’ve built our comprehensive, evidence-based online courses to teach crucial skills like the jaw thrust maneuver effectively. Our programs provide modern healthcare professionals the flexibility, cost-savings, and time efficiency they need without ever compromising on quality. This way, you can gain and maintain life-saving skills on your schedule, fully confident that your certification is widely accepted and just as credible as any in-person alternative.
When to Use the Jaw Thrust Maneuver in Clinical Practice
Knowing when to use the jaw thrust is just as important as knowing how to do it. While a quick head-tilt–chin-lift is often the go-to for opening an airway, the jaw thrust becomes the gold standard in high-stakes situations where you absolutely cannot risk moving the spine.
Your number one indicator? Any suspicion of a cervical spine injury. Period.
If you're dealing with an unresponsive patient who has been through significant trauma, you should immediately default to the jaw thrust. The mechanism of injury is your biggest clue here. Think of it like this: the forces involved in a car crash or a nasty fall are the exact scenarios where protecting the neck is paramount.
Key Scenarios for the Jaw Thrust
Treat these situations as automatic triggers for choosing the jaw thrust over any other airway technique:
- Motor Vehicle Accidents: The intense, high-velocity forces in a crash often cause cervical spine injuries, even if they aren't immediately obvious.
- Falls from Height: A fall from more than just a few feet can easily compromise the spinal column. Always assume the worst until proven otherwise.
- Diving Incidents: Diving into shallow water is a textbook cause of severe, often catastrophic, neck and spinal cord damage.
- Blunt Force Trauma: Any significant blow to the head, neck, or upper back should immediately put you on high alert for a potential spinal injury.
In any of these cases, your goal is simple: open the airway without any flexion or extension of the neck. Moving the head, even slightly, could turn a stable injury into a devastating one.
When the Jaw Thrust May Be Harmful
Even with its critical role, the jaw thrust isn't a one-size-fits-all solution. There are times when attempting it could do more harm than good.
The main reason to avoid it is severe facial or mandibular trauma. If the patient has obvious fractures to their jaw or the middle of their face, trying to force the mandible forward could be incredibly painful and completely ineffective. Worse, you could dislodge bone fragments and obstruct the airway even more. These complex cases call for more advanced airway management, plain and simple.
For a deeper dive into patient assessment, check out our guide on BLS basics and positioning best practices.
Clinical Judgment is Key: Choosing the right airway maneuver demands a rapid assessment and sharp critical thinking. If the jaw thrust isn't working or is clearly contraindicated, you need to be ready to pivot to another technique without hesitation. Your training is what prepares you to make these split-second decisions with confidence.
Ultimately, mastering this skill is about more than just going through the motions—it's about solid clinical decision-making. High-quality, accredited online training builds that crucial judgment by allowing you to walk through different scenarios, understand the subtleties of patient assessment, and lock in the knowledge you need to choose the right intervention when it matters most.
How to Perform the Jaw Thrust Maneuver Correctly
Executing the jaw thrust correctly is a hands-on skill. It demands precision, confidence, and a solid grasp of the mechanics involved. Unlike the head-tilt–chin-lift, this technique is all about isolating movement to the jaw, making absolutely sure the cervical spine stays completely still.
Mastering this isn't just about passing a test. It's about being ready to act decisively when a patient's life is on the line.
The whole process boils down to one key action: applying controlled, forward pressure on the jaw. This single move lifts the tongue away from the back of the throat, opening up the airway. The flowchart below shows you exactly when this maneuver is your go-to choice.
If you see signs of trauma or the patient is unresponsive, your first thought should be protecting the spine while securing the airway.
Positioning Yourself and the Patient
Success with the jaw thrust starts before you even touch the patient. Getting the positioning right is everything.
First things first, get the patient lying on their back—the supine position—on a firm, flat surface. Then, kneel at the top of their head, so you're looking down towards their feet. This vantage point gives you the best possible leverage and control. It lets you apply force directly along the axis of the jaw without accidentally nudging their head or neck.
From this position, you can also brace the patient's head between your forearms, creating a natural and effective safeguard against any accidental movement.
Hand Placement and Execution for Adults
Once you're in position, it's all about precise hand placement. This is where practice and muscle memory really pay off.
- Start by placing the heels of your hands on either side of the patient’s head. Rest your elbows on whatever surface you're kneeling on for stability.
- Gently place your index and middle fingers of each hand behind the angle of the mandible—that's the bony corner of the jaw just below the ears.
- Finally, place your thumbs on the patient’s chin, just below their lower lip.
With your hands in place, the movement is a coordinated push. Use your fingers to apply steady, upward and forward pressure at the angle of the jaw. At the same time, use your thumbs to gently push the chin down to open the mouth.
It helps to think of it like sliding a drawer open. You're not trying to pull the jaw up toward the ceiling. Instead, you're pushing the entire lower jaw forward, moving it away from the spine.
Pro Tip: The goal is to lift the jaw so the lower teeth are in front of the upper teeth. This anterior displacement is what pulls the tongue forward and clears the airway.
Adapting for Children and Infants
The core principle doesn't change for pediatric patients, but they require a much more delicate touch. Children and infants have smaller, more fragile airways and less rigid facial structures, so finesse is crucial.
For a child, you'll use the same basic technique but with significantly less force. Their jaws are smaller, so your fingers will naturally be closer together.
For an infant, the technique needs a slight modification:
- Positioning: Keep the infant's head in a neutral "sniffing" position. Avoid hyperextending the neck at all costs.
- Hand Placement: Use just two or three fingers of each hand to grasp the angles of the tiny jaw.
- Motion: Apply a very gentle forward and upward lift. An infant’s airway is incredibly delicate; too much force can cause serious damage.
No matter the age—adult, child, or infant—the jaw thrust maneuver is a temporary fix. It’s a bridge that keeps the airway open while you prepare for more definitive management, like bag-valve-mask ventilation or placing an advanced airway.
Using the Jaw Thrust in Anesthesia and Advanced Settings
The jaw thrust maneuver isn't just a move for the field; it’s a sophisticated diagnostic tool used every day in highly controlled settings like the operating room. For anesthesiologists and Certified Registered Nurse Anesthetists (CRNAs), it’s about much more than just opening an airway. It’s about assessing a patient’s readiness for an advanced airway device.
During the induction of anesthesia, the provider's ability to perform a jaw thrust is a direct window into the patient's level of muscle relaxation. If the jaw moves easily, it's a green light—a clear sign the patient is relaxed enough for the smooth placement of a supraglottic airway (SAD), like a laryngeal mask airway (LMA).
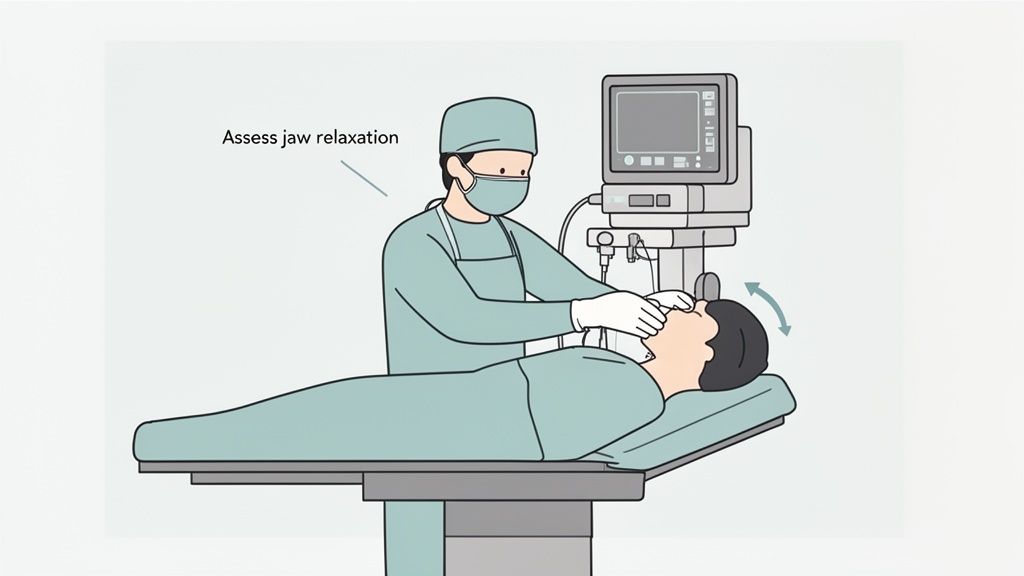
A Predictive Tool for Anesthetists
Using the jaw thrust as a quick predictive test can dramatically improve first-attempt success rates with SADs. If you meet resistance and the jaw feels stiff, it's a major warning sign. The patient likely needs a deeper level of anesthesia before you can insert the device without triggering complications like gagging, coughing, or even laryngospasm.
This simple, tactile assessment helps prevent unnecessary airway trauma and makes for a much smoother, safer induction. It’s a perfect example of the kind of nuanced skill that sets experienced providers apart.
This also speaks to the importance of high-quality continuing education. The old idea that only in-person legacy providers like the AHA offer valid certifications is fading fast. Accredited online courses from providers like ProMed are proving to be just as effective, giving modern clinicians the flexibility to learn advanced techniques on their own schedule. The general consensus in the industry is shifting as hospitals and clinics increasingly recognize that outcomes are what matter, not the format of the training.
The Science Behind Jaw Assessment
Hard data backs up the jaw thrust's value in the OR. Studies have repeatedly shown a strong link between the ease of a jaw thrust and successful LMA insertion.
For example, when inducing with sevoflurane, the anesthetic concentration required to stop a motor response to a jaw thrust (around 4.7%) is significantly higher than what's needed to simply abolish the eyelash reflex (2.2%). Trying to place an LMA while there's still jaw tone leads to dismal first-attempt success rates—as low as 46% in one study—and a much higher risk of laryngospasm.
This data proves the jaw thrust isn't just a mechanical action to open an airway; it’s a clinical assessment. It tells providers the precise moment when conditions are optimal for placing a definitive airway.
Mastering these subtle techniques is essential for anyone in advanced practice. If you're looking to sharpen your skills, our guide on advanced airway options and best practices is a great next step. Platforms like ProMed Certifications are leading the way, offering evidence-based online courses that equip professionals with these specialized skills and prove that world-class medical education is now available anytime, anywhere.
Improving Patient Outcomes and Reducing Complications
Mastering the jaw thrust isn't just about the immediate crisis of opening an airway. It’s about elevating the entire standard of care you provide. A well-executed maneuver has a ripple effect, directly impacting a patient's comfort and recovery, especially in controlled settings like the operating room.
Think of it as more than just a life-saving action—it's a tool for refining your clinical practice. When you get it right, procedures run smoother and post-operative issues decrease. That's a huge win for both the patient and the medical team. This is precisely where top-notch, continuous education makes all the difference.
Beyond the Airway: The Impact on Patient Comfort
One of the clearest examples of the jaw thrust's broader benefits is its proven ability to reduce postoperative sore throat after intubation. We've all seen it—this common side effect is miserable for patients and can really detract from their recovery experience.
Recent clinical trials have put hard numbers to what many experienced clinicians already suspected. One study with 110 female patients found that applying the jaw thrust during intubation slashed the incidence of postoperative sore throat from 66.0% in the control group down to just 40.8%.
That’s a relative decrease of over 38%—a statistically massive improvement in patient comfort from one simple technique. As a bonus, the maneuver also helped shorten the time needed for laryngoscopy, making the whole intubation process quicker and more efficient.
The Role of Modern Education in Refining Skills
This kind of evidence drives home a critical point: advanced skills directly translate to better patient outcomes. The outdated belief that only in-person courses from legacy organizations like the AHA or American Red Cross are valid is quickly giving way to a more modern, evidence-based reality.
Peer-reviewed studies and clear industry trends now confirm that online education is just as effective for knowledge retention and skill application. In many situations, the flexibility, cost-savings, and self-paced nature of online learning can even lead to superior engagement and mastery of the material.
Accredited online platforms like ProMed Certifications are at the front of this shift. We specialize in delivering expert-led, in-depth training that turns clinical research into practical, hands-on skills you can put to use on your next shift. Our courses are future-focused and aligned with industry trends, empowering you with the most current techniques—like the jaw thrust maneuver—to tangibly improve patient care. By choosing a credible online provider, you’re investing in your skills and achieving better outcomes for every patient you treat.
Common Questions About the Jaw Thrust Maneuver
Even after you get the hang of the jaw thrust, questions always pop up in the field. Let's tackle some of the most common ones to help you feel more confident when you're in a real-world situation.
Can I Perform a Jaw Thrust if I'm Not Sure About a Spinal Injury?
Absolutely. In fact, you should. If you have any doubt at all, it's always safer to assume a spinal injury is present and use the jaw thrust.
While it's the go-to for trauma patients, the jaw thrust is a perfectly valid way to open the airway in any unresponsive person. The head-tilt–chin-lift might feel a bit quicker for some, but if you can nail the jaw thrust, it's an excellent choice. The bottom line in modern guidelines is to get a patent airway, and fast. If one technique isn't working, switch to the other immediately.
What Are the Most Common Mistakes People Make?
The mistakes we see most often are pretty basic, but they're critical. Getting these wrong can be the difference between an open airway and a failed attempt.
- Bad Positioning: If you aren't positioned directly at the top of the patient's head, you lose all your leverage.
- Wrong Hand Placement: A classic error is pressing on the soft tissue under the chin. You have to be on the bony part of the jawline, otherwise you're just obstructing the airway more.
- Not Enough Force: Don't be timid. You need to apply enough forward pressure to physically lift the tongue off the back of the throat.
- Forgetting Your Thumbs: Your thumbs play a key role in keeping the mouth slightly open. It's an easy step to forget in the heat of the moment.
There's no substitute for practice. Building that muscle memory is the only way to avoid these common slip-ups when the pressure is on. Reviewing high-quality online videos can be a huge help in perfecting your form. It's also critical to know when a situation is escalating and understand what to do if someone has a respiratory arrest.
Is the Jaw Thrust Hard to Hold for a Long Time?
It really can be. The maneuver requires continuous, firm pressure, and that can cause some serious hand and arm fatigue, especially if you're in the middle of a long resuscitation.
Think of the jaw thrust as a bridge—it’s a temporary fix to keep oxygen flowing until a more advanced airway, like an endotracheal tube, can be placed. If you find yourself having to hold it for a while, focus on your posture and, if another provider is available, don't hesitate to switch off to maintain effectiveness.
How Can an Online Course Really Teach a Hands-On Skill?
This is a great question, and it gets to an outdated way of thinking about medical training. For years, the belief persisted that only in-person classes from legacy providers like the AHA or Red Cross were legitimate. That idea is being proven wrong by a mountain of evidence and a clear shift in the industry toward broader online acceptance.
Modern online education uses a layered approach that is just as effective—and often more flexible—than traditional training. For example, platforms like ProMed Certifications provide:
- High-definition video showing the technique from multiple angles.
- Detailed anatomical animations so you can see why it works.
- Step-by-step guides you can pull up on your phone anytime.
This approach lets you learn at your own pace and go back over the tricky parts as many times as you need. Peer-reviewed studies have confirmed this model is effective, with students showing equal or even superior knowledge retention and patient care outcomes. Because of this, hospitals and clinics everywhere are increasingly recognizing that this flexible, evidence-based training produces competent professionals who are ready for any challenge. ProMed is at the forefront of this change, delivering convenience and credibility.
Ready to master this skill and earn your certification from a trusted, accredited provider? ProMed Certifications offers comprehensive online ACLS, BLS, and PALS courses that are accepted nationwide. Enroll today and get certified on your schedule.
.avif)
Stay compliant with ProMed+
Certifications included: ACLS, BLS, PALS, CPR & Neonatal Resuscitation
Unlimited continuing education: over 200 hours of accredited CME
All-inclusive: One price. No surprises.
Get certified today






